Can You Drive After a Steroid Injection?
Summary:
-
If in doubt, arrange someone to drive you.
-
Many people feel fine, but short-term effects (dizziness, numbness, weakness, pain flare) can impair safe driving.
-
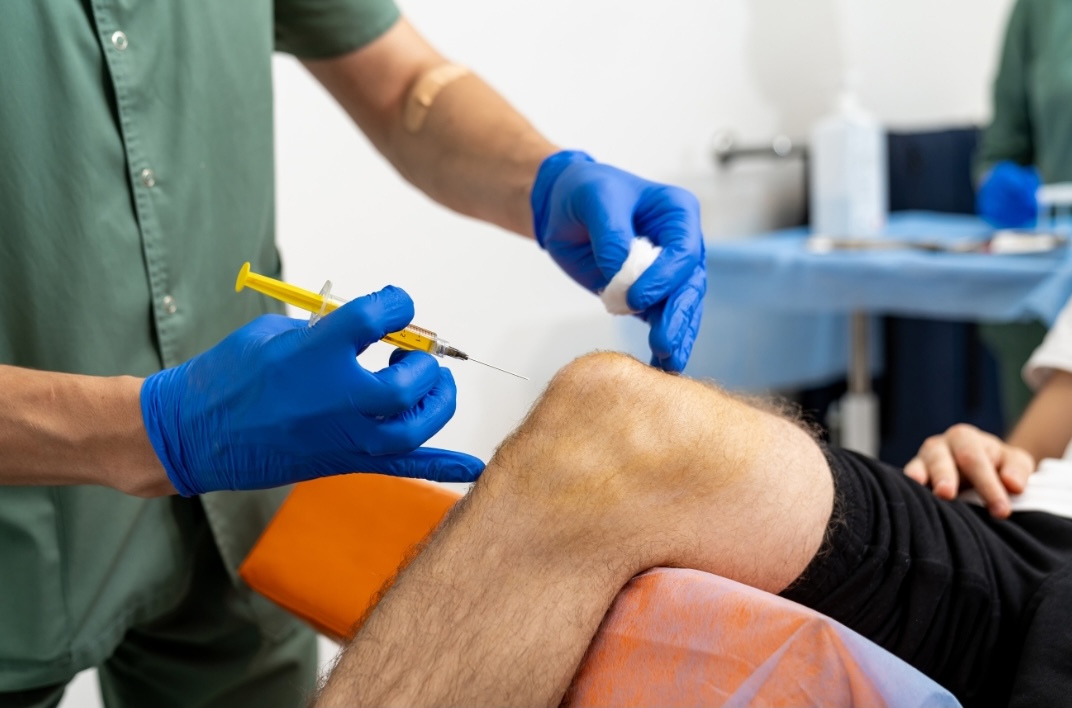
Lower-limb injections (hip, knee, foot) are more likely to affect pedal control.
-
Wait at least 15 minutes post-procedure to ensure symptoms settle; longer if you feel off.
-
Insurance could be at risk if you drive while impaired.
-
Sonoscope’s Hertfordshire clinics provide ultrasound-guided injections and personalised aftercare advice.
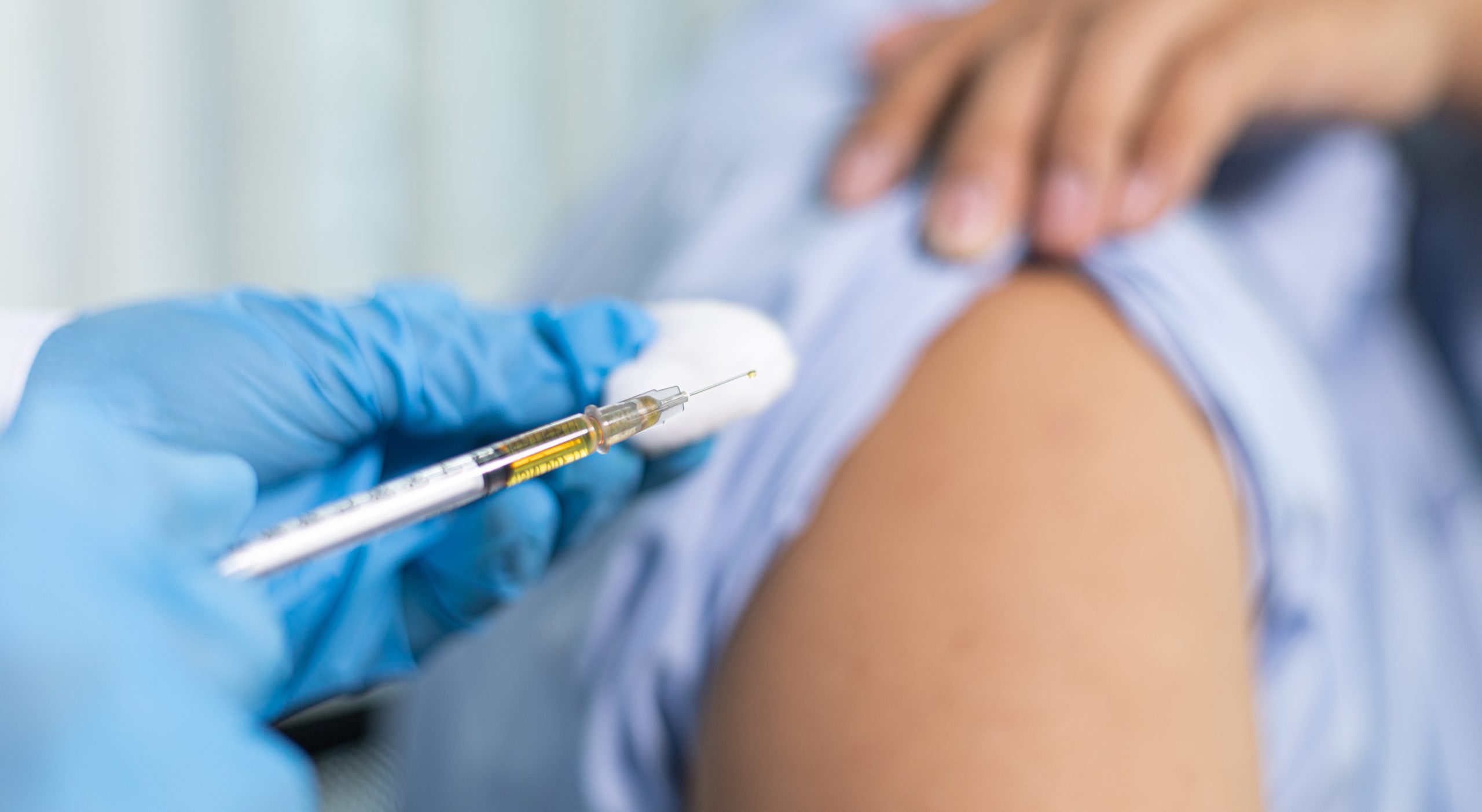
Steroid injections are a common and effective way to reduce pain and inflammation, especially when guided by ultrasound for precision. The general advice is to be as safe as possible and, if you’re unsure, bring someone to drive you. Many people are unaffected by a steroid or local anaesthetic injection, but understanding potential side effects helps you make a balanced, informed decision.
Why Driving After a Steroid Injection May Be Risky
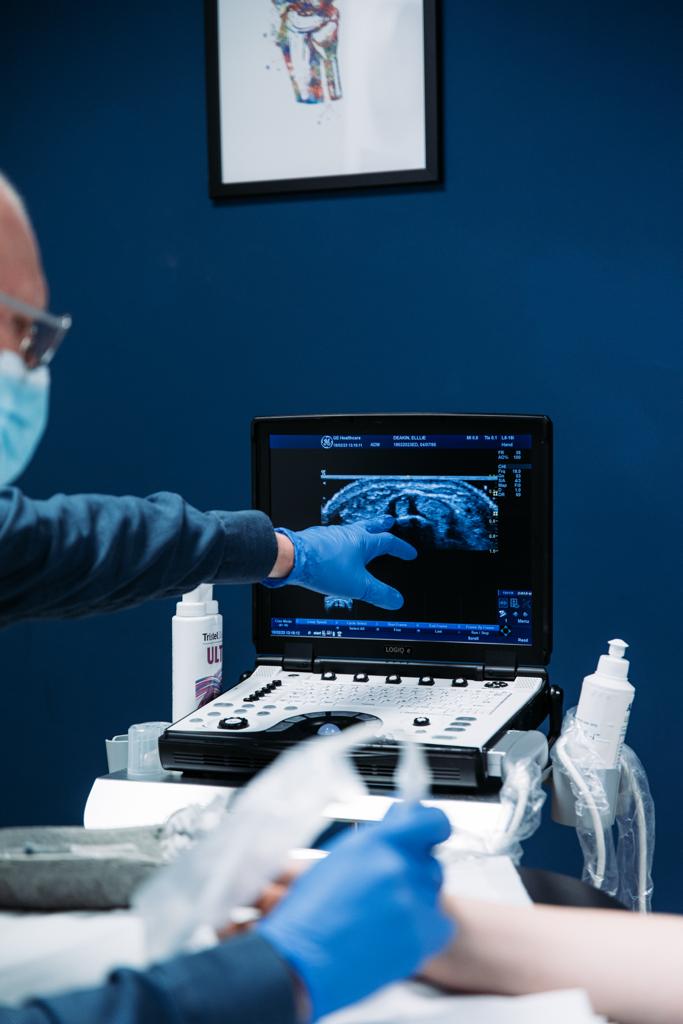
Short-term effects can affect your ability to drive safely. Possible symptoms following a steroid or local anaesthetic injection include dizziness or light-headedness, temporary weakness or numbness near the injected area, and a general feeling of unsteadiness or fatigue. At Sonoscope’s Hertfordshire ultrasound-guided injection clinics, patients are usually advised to stay in the waiting area for around 15 minutes after the procedure to ensure any temporary side effects have settled before travelling home.
The Effects of Local Anaesthetic
Many steroid injections include a local anaesthetic to numb the area. This can cause temporary numbness, weakness, or altered sensation, particularly if the injection site involves muscles or joints used for driving. If you notice reduced control or sensitivity, do not drive until normal function returns.

Location of Injection Matters
Injections in the lower limbs, such as the hip, knee, or foot, can temporarily affect your ability to operate the pedals for accelerating and braking. If your injection was in these areas, it’s safest to arrange for someone to drive you home or use alternative transport.
Post-Injection Flare
A temporary increase in pain, known as a “steroid flare,” can occur within the first 24 to 48 hours after the injection. This sudden pain can be distracting and may reduce your ability to react quickly, particularly if you need to perform an emergency stop. If you experience a flare, postpone driving until symptoms settle.
Insurance and Legal Considerations
Some insurance policies may not cover you if you drive while impaired after a medical procedure. If you were involved in an accident and it was determined that the injection affected your ability to drive, your insurance could be invalidated. Check your policy, and if you’re unsure, err on the side of caution and avoid driving.
Professional Guidance and Aftercare
At Sonoscope, our clinicians provide ultrasound-guided steroid injections with personalised aftercare to support a safe recovery. If you’re in Hertfordshire and have questions about driving, working, or exercising after an injection, our musculoskeletal specialists can advise based on your condition and the injection site.
Bottom Line
If you feel dizzy, weak, numb, unusually sore, or even just uncertain about your control or concentration, don’t drive. Wait until you feel fully capable, or arrange a lift. Your safety, and the safety of others, comes first.
Ready to speak with a clinician?
Sonoscope provides ultrasound-guided steroid injections across Hertfordshire. Book online or call us on 07999 923 844.
For more information on treatment costs you can explore the full breakdown of private ultrasound-guided injection prices across our Hertfordshire clinics here.
Frozen shoulder and injection therapy
What is a frozen shoulder (Adhesive Capsulitis)?
Frozen shoulder is a condition that can cause the shoulder to become very painful and stiff. Frequently there is no clear reason as to why frozen shoulder comes on. Sometimes people can remember a particular trigger like holding themselves steady on a bus when its suddenly breaks and the arm is jerked. Or tripping or very rapidly moving the shoulder to break a fall etc.
At the time these incidents are often not thought to be that serious but sometimes it sets in motion the early stages of what eventually will become clear as the early stages of frozen shoulder or adhesive capsulitis. Frozen shoulder often affects people in the 40s to 60s. The highest incidence is seen in those in their 50s.
What are the early symptoms of frozen shoulder?
Pain symptoms: The pain is often described as a dull ache in the shoulder. Initially can be perceived as mild but over time it can become more intense. Usually the pain is worse at night. The pain usually is of a gradual onset. The pain often progresses from the initial ache to a more severe pain.
Stiffness: Initially people might find there are subtle restrictions in range of motion. It might be noticed that reaching higher up or putting on a coat feels like more of an effort.
Traditionally three different stages are described in literature.
The freezing stage. Where pain is gradually intensified as time goes by. The shoulder also become stiffer during that period.
The frozen stage when the stiffness is quite significant but pain levels are actually slightly less intense
The thawing stage which is the recovery phase when slowly movement is regained and pain subsides.
Who are most at risk of frozen shoulder?
People between 40 and 60 are more likely to be affected.
People who suffer from diabetes are more likely to be affected.
People who have thyroid disorders are also more likely to be affected.
How if frozen shoulder diagnosed?
Frozen shoulder is primarily a clinical diagnosis. A detailed history and detailed clinical examination is usually enough to make the diagnosis.
There are a number of other conditions that can have features consistent with frozen shoulder. Some of these conditions are listed below:
- Osteoarthritis of the glenohumeral joint
- Rotator cuff impingement syndrome
- Calcific tendinopathy
- Osteoarthritis of the acromioclavicular (AC) joint
- Long head of biceps tendinopathy
Imaging investigations to further investigate the painful shoulder
X-ray:
In order to evaluate the bony anatomy i.e. check it to see if there is any degenerative change or bony trauma such as fracture an x-ray is an excellent imaging option.
Diagnostic Ultrasound:
In order to evaluate the soft tissues such as musculature including tendon and ligaments as well as nerves as well as blood vessels real time investigation such as diagnostic ultrasound is fantastic. Ultrasound is however operator dependent and therefore requires a very skilled operator to carry out. The resolution of high-resolution ultrasound is higher then MRI.
MRI scan:
For most common shoulder condition MRI is not required as bone and soft tissue can be evaluated very well with ultrasound and as indicated perhaps at times x-ray. Of course there are some conditions where MRI might be required and at Sonoscope we always guide you in this direction when this is the case.
What injection options do we have for frozen shoulder?
For all frozen shoulders we would advise people to have a steroid injection. However especially in cases where the shoulder is very restricted it could be even more beneficial to have a hydrodistention injection. Which is a combination of steroid and a volume of (salty) water.
Steroid injection:
Steroid injection is very effective (Sun et al, 2017) in reducing inflammation and improving function . As inflammation drives frozen shoulder has steroid injection inside of the shoulder joint is therefore very good at very rapidly reducing high levels of inflammation and pain. Once pain levels have reduced these people can then with the help of further physiotherapy and or exercise focused management fully recover functionally.
Hydrodilatation/Hydrodistension:
The steroid is injected with a volume of local anaesthetic and then a further volume (possibly as much as 30 mL) of saline. The volume of the injection stretches the joint capsule which helps to restore flexibility of the shoulder joint. Evidence (Lin et al., 2018) does demonstrate that hydrodistention injections are more effective in improvement of external rotation of the shoulder than regular steroid injection.
https://www.youtube.com/watch?v=skvaSCCcfHI
Number of steroid injections required:
In most cases one injection is sufficient to make a good recovery. However in some cases after several months there is a degree of recurrence and then another injection might be required.
Please contact us on: 07999 923844 to book an appointment or email us at: info@sonoscope.co.uk
Lin, M.T., Hsiao, M.Y., Tu, Y.K. and Wang, T.G., 2018. Comparative efficacy of intra-articular steroid injection and distension in patients with frozen shoulder: a systematic review and network meta-analysis. Archives of physical medicine and rehabilitation, 99(7), pp.1383-1394.
Sun, Y., Zhang, P., Liu, S., Li, H., Jiang, J., Chen, S. and Chen, J., 2017. Intra-articular steroid injection for frozen shoulder: a systematic review and meta-analysis of randomized controlled trials with trial sequential analysis. The American journal of sports medicine, 45(9), pp.2171-2179.
Iliopsoas Tendinopathy/ Iliopsoas Bursitis - Ultrasound Guided Injections
Iliopsoas tendinopathy / bursitis what is it?
Iliopsoas tendinopathy affects the iliopsoas tendon which is an important hip flexor and stabiliser muscle attaching to the lumbar spine and pelvis as well as the femur (thigh bone).
When the tendon becomes irritated and inflamed it can swell up and become chronically inflamed and irritated which we do call a tendinopathy. This problem usually occurs due to repetitive activity which can include running. In the process it can also cause inflammation to the bursa which is small fluid sac that is normally almost empty and lies adjacent to the tendon but can then swell up and become painful which is called an iliopsoas bursitis.
Ultrasound-guided steroid injections can be very useful in specifically targeting this tendon and/or bursa. This of course is to get pain levels under control and once symptoms have diminished then further physiotherapy input and/or other conditioning work is very important to obtain long-term improvement.

What are the symptoms of Psoas Tendinopathy/Bursitis?
Symptoms can vary but usually symptoms have the following components:
- Pain that is felt over the anterior hip area. Oftentimes this is a deep ache but in other cases it could be very sharp pain.
- A clicking or snapping sensation. As the tendon moves over the inflamed hip/bursa sometimes a snapping or clicking sensation can be noticed during movements.
- Due to significant pain there might be limitation in range of motion of the hip as well.
- In almost all cases there is a very specific local pain area that patients often time can point to by pressing on it.
Conditions that can be confused with Iliopsoas Tendinopathy/Bursitis:
There are a number of other conditions that can also present as iliopsoas tendinopathy or bursitis. Please see below a number of common conditions that can refer pain in his region:
- A deep aching pain in the groin area is often common in people with osteoarthritis of the hip joint.
- Disorders of the lumbar spine such as spinal stenosis or a herniated intervertebral disc can also refer pain in the anterior hip region.
- Other conditions such as Gilmore’s groin (sports hernia) or adductor tendinopathy can also present with pain in this anterior hip region.
- Pain at the more lateral aspect of the hip (at the side of the hip) is often due to greater trochanteric pain which is related to gluteal tendon insertional tendinopathy or greater trochanteric bursitis.
What are the main causes of iliopsoas tendinopathy/bursitis?
Iliopsoas bursitis and iliopsoas tendinopathy are relatively uncommon conditions. In clinical practice when people present with anterior hip pain this condition is over diagnosed. Very few people after further investigation (ultrasound or MRI) appear to have genuine iliopsoas tendinitis or bursitis.
- Overuse and repetitive activities are one of the main two causes of iliopsoas bursitis. Activities such as running kicking sports such as kickboxing cycling can all cause inflammation.
- The main other category is that of joint specific conditions such as osteoarthritis, rheumatoid arthritis which due to enlargement and osteophyte formation can cause irritation of the iliopsoas bursa and tendon.
How is iliopsoas tendinopathy/bursitis diagnosed? (How do I know that I have iliopsoas tendinopathy/bursitis?)
Clinical examination alone (examination of the hip looking for range of motion in the hip strength of the hip musculature and also local palpation of the painful area) is not enough to come to the definitive conclusion of iliopsoas tendinopathy or bursitis.
Further imaging is required to get more definitive clarity on a diagnosis.
Diagnostic ultrasound
Is often very helpful to identify features of osteoarthritis. It of course can evaluate in detail the iliopsoas tendon itself and any bursitis that might be there as well as other tendon and muscle structures in the region.
At Sonoscope you will not only receive a detailed clinical examination but in addition to that a diagnostic ultrasound all within the same session which Is very important to come to a diagnosis.
X-rays
Can be very helpful to identify degenerative changes such as osteoarthritis where x-ray is very helpful for as it is very good depicting bone and can demonstrate any narrowing of the joint space which indicates lack of cartilage and through that the degree of degenerative changes that are present in the hip.
MRI imaging
As the hip joint is a complex three-dimensional structure and in the femoral head is in the deep socket (the acetabulum) is therefore difficult to evaluate the structure deep within the socket.
MRI is very good as it takes multiplanar images at very small slices which is very sensitive in evaluating soft tissues such as the labrum muscles as well as tendons. Patient has to remain still during the examination which can take half an hour to an hour. Samurai is also very good at evaluating the bone structures as well.
Some of the drawbacks of MRI is that some people find being in a small confined space very claustrophobic and cannot therefore endure being in an MRI scanner. Some people do have existing metal work from potentially from previous surgery and this can cause significant artefact and difficulty in evaluating the tissue surrounding it. Pacemakers can only be taken into MRI scanners that are pacemaker safe which is not the case with every scanner
.
Ultrasound-guided steroid injection
Ultrasound-guided steroid injections are very accurate when targeting structures such as iliopsoas tendon and iliopsoas bursitis.
During the procedure a small amount of steroid plus local anaesthetic will be injected either adjacent to the tendon or in the iliopsoas bursa. The use of ultrasound guidance also improves the safety of this injection and can help reduce unnecessary pain by avoiding pain sensitive structures. Steroid injections vary in the length of time that they can provide pain relief ranging from a few months to a year or more. Most people will at least get two to three months of pain relief,

At Sonoscope we offer a One-Stop-Clinic. This includes: consultation and clinical examination, a diagnostic ultrasound and if appropriate also an ultrasound-guided injection which in the case of iliopsoas tendinopathy or iliopsoas bursitis is a steroid injection.
For any further information and or if you want to book an appointment then please call us on: 07999 923844 or email us about info at info@sonoscope.co.uk
Does a steroid injection make you put on weight?
So the answer to this question is no.
But it is possible for people to put on weight with long-term steroid use, but this is related to the use of oral steroids (tablets). This does not apply to steroid injections for use for structures such as joints or tendons.
What is the difference between steroid tablets and steroid injections?
Steroid injections used to treat tendon inflammation or joint inflammation are specifically targeted to work at a local level, i.e., at the site of injection and not elsewhere. As the steroid dosage is relatively low, for most musculoskeletal conditions the maximum dosage is 40 mg and the minimum dosage is 10 mg. These dosages of steroids do not have an impact on the overall body metabolism and only have minimal systemic absorption.
In addition to that, we only administer steroid injections under ultrasound guidance, which means that the steroid is targeted very specifically, which further helps to reduce unnecessary spread of the steroid to areas where it is not required or needed.
Steroids such as prednisolone, however, are used for many other conditions, such as autoimmune conditions like rheumatoid arthritis and systemic lupus erythematosus (SLE), as well as inflammatory bowel disease. It is also often used in respiratory conditions such as asthma and COPD as well as part of a treatment regime in certain types of cancer such as leukaemia and lymphoma. For these conditions, steroid dosages are often much higher and taken for longer periods of time, which in some cases can lead to significant weight gain.
Can steroid injections lead to weight gain?
Steroid injections as used at Sonoscope are for musculoskeletal conditions and do not lead to weight gain. As explained above, the dosages are much smaller than those used by people with certain medical conditions that require taking steroid tablets for longer periods of time.
There are a number of studies that have clearly demonstrated that people can put on weight when using steroids over the longer term. One study found that 10.2% of individuals exposed to steroids chronically experienced weight gain of at least 10% or more of their usual weight. The risk was higher for younger people, smokers, women and people on high dosages of steroids (Fardet et al., 2021).
Which steroids do we inject?
Generally for musculoskeletal conditions, mostly two types of steroids are used in the UK: Depo Medrone (methylprednisolone) is the most used steroid, closely followed by Triamcinolone Acetonide (Kenalog). At the time of speaking, Triamcinolone Acetonide (Kenalog) is now discontinued by the manufacturer, and any remaining stocks are expected to be exhausted by early June 2025.
At Sonoscope we inject Depo-Medrone. Some hyaluronic acid products come premixed with steroids already, such as a product called Cingal, which comes with Triamcinolone hexacetonide, a long-acting steroid which is not available to purchase on its own in the UK.
Which conditions are steroid injections generally used for?
Common conditions for which we use steroid injections and sonoscope are osteoarthritis of the knees, frozen shoulder, tennis elbow, carpal tunnel syndrome, etc.
Other common conditions that we also inject are: Trigger finger as well as a number of joints that are affected by osteoarthritis, such as osteoarthritis of the wrist and hand, osteoarthritis of the elbow, osteoarthritis of the shoulder osteoarthritis of the ankle and osteoarthritis of any of the foot joints.
Other conditions that we inject under ultrasound guidance: De Quervain’s tenosynovitis, ganglion cysts around the wrist and fingers. Golfers elbow, olecranon bursitis, subacromial bursitis in the shoulder, trochanteric bursitis at the hip, iliopsoas bursitis at the hip, insertional tendinopathy at the hamstring, Morton’s neuroma at the foot, aspiration of Baker’s cyst at the back of the knee.
So the answer to this question is no.
But it is possible for people to put on weight with long-term steroid use, but this is related to the use of oral steroids (tablets). This does not apply to steroid injections for use for structures such as joints or tendons.
What is the difference between steroid tablets and steroid injections?
Steroid injections used to treat tendon inflammation or joint inflammation are specifically targeted to work at a local level, i.e., at the site of injection and not elsewhere. As the steroid dosage is relatively low, for most musculoskeletal conditions the maximum dosage is 40 mg and the minimum dosage is 10 mg. These dosages of steroids do not have an impact on the overall body metabolism and only have minimal systemic absorption.
In addition to that, we only administer steroid injections under ultrasound guidance, which means that the steroid is targeted very specifically, which further helps to reduce unnecessary spread of the steroid to areas where it is not required or needed.
Steroids such as prednisolone, however, are used for many other conditions, such as autoimmune conditions like rheumatoid arthritis and systemic lupus erythematosus (SLE), as well as inflammatory bowel disease. It is also often used in respiratory conditions such as asthma and COPD as well as part of a treatment regime in certain types of cancer such as leukaemia and lymphoma. For these conditions, steroid dosages are often much higher and taken for longer periods of time, which in some cases can lead to significant weight gain.
Can steroid injections lead to weight gain?
Steroid injections as used at Sonoscope are for musculoskeletal conditions and do not lead to weight gain. As explained above, the dosages are much smaller than those used by people with certain medical conditions that require taking steroid tablets for longer periods of time.
There are a number of studies that have clearly demonstrated that people can put on weight when using steroids over the longer term. One study found that 10.2% of individuals exposed to steroids chronically experienced weight gain of at least 10% or more of their usual weight. The risk was higher for younger people, smokers, women and people on high dosages of steroids (Fardet et al., 2021).
Which steroids do we inject?
Generally for musculoskeletal conditions, mostly two types of steroids are used in the UK: Depo Medrone (methylprednisolone) is the most used steroid, closely followed by Triamcinolone Acetonide (Kenalog). At the time of speaking, Triamcinolone Acetonide (Kenalog) is now discontinued by the manufacturer, and any remaining stocks are expected to be exhausted by early June 2025.
At Sonoscope we inject Depo-Medrone. Some hyaluronic acid products come premixed with steroids already, such as a product called Cingal, which comes with Triamcinolone hexacetonide, a long-acting steroid which is not available to purchase on its own in the UK.
Which conditions are steroid injections generally used for?
Common conditions for which we use steroid injections and sonoscope are osteoarthritis of the knees, frozen shoulder, tennis elbow, carpal tunnel syndrome, etc.
Other common conditions that we also inject are: Trigger finger as well as a number of joints that are affected by osteoarthritis, such as osteoarthritis of the wrist and hand, osteoarthritis of the elbow, osteoarthritis of the shoulder osteoarthritis of the ankle and osteoarthritis of any of the foot joints.
Other conditions that we inject under ultrasound guidance: De Quervain’s tenosynovitis, ganglion cysts around the wrist and fingers. Golfers elbow, olecranon bursitis, subacromial bursitis in the shoulder, trochanteric bursitis at the hip, iliopsoas bursitis at the hip, insertional tendinopathy at the hamstring, Morton’s neuroma at the foot, aspiration of Baker’s cyst at the back of the knee.
ITB friction syndrome
IT Band Syndrome, also called Iliotibial Band Syndrome, is a frequent overuse injury in athletes, especially runners and cyclists. This condition arises when the iliotibial band, a thick tissue band running along the outside of the thigh from the hip to the knee, becomes tight or inflamed. It can lead to considerable pain and impede performance.
Effective treatment is essential for recovery and preventing further injury. In the first instance, physiotherapy is the mainstay of treatment.
The treatment will involve:
- Rest, Ice, stretching exercises
- Specific exercises targeting the muscles supporting the hip and knee in particular
- Adjusting training load
- Taping of the knee
- Biomechanical assessment of running technique and modification
- Soft tissue manipulation
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
If symptoms are persistent or severe and physiotherapy is not making any impact on symptoms, then injection therapy is the next step to deal with this condition effectively. Sonoscope offers pinpoint accurate ultrasound-guided injections directly targeting the structure affected.
How Is IT Band Syndrome Diagnosed?
How is IT Band Syndrome diagnosed? This is an important question, especially if you are experiencing pain on the outside of your knee. IT Band Syndrome, or Iliotibial Band Syndrome, is a common injury among runners and other athletes. The iliotibial band is a thick band of tissue that runs along the outside of your thigh, from your hip to your knee. When this band becomes tight or inflamed, it can cause pain and discomfort, especially during physical activities.
The first step in diagnosing IT Band Syndrome is usually a visit to a doctor or a physical therapist. They will start by asking you about your symptoms and your medical history. They will want to know when the pain started, where exactly it hurts, and what activities seem to make it worse. They will also ask about your exercise routine and any recent changes in your activity level.
Next, the doctor will perform a physical examination. They will look at your leg and knee, checking for areas of tenderness and swelling. They may press on the outside of your knee to see if it is painful. They will also observe your posture and gait to see if there are any abnormalities that could be contributing to your symptoms.
In addition to the physical examination, the doctor may ask you to perform certain movements or exercises. These tests are designed to put stress on the iliotibial band and see if they reproduce your symptoms. For example, they might ask you to bend and straighten your knee while pressing on the outside of it. If this causes pain, it could be a sign of IT Band Syndrome.
Sometimes, imaging tests may be used to help diagnose IT Band Syndrome. An X-ray can rule out other conditions that might be causing your knee pain, such as a fracture or osteoarthritis. An MRI (Magnetic Resonance Imaging) scan can provide a detailed image of the soft tissues in your leg, including the iliotibial band. This can help to confirm the diagnosis and rule out other possible causes of your symptoms.
However, imaging is not always necessary for diagnosing IT Band Syndrome. In many cases, a thorough history and physical examination is enough to make the diagnosis. The doctor or physical therapist will then discuss the findings with you and explain the next steps for treatment.
In summary, diagnosing IT Band Syndrome involves a combination of taking a medical history, performing a physical examination, and sometimes using imaging tests. The key to successful treatment and prevention is to address the underlying causes and make necessary changes to your activity routine. If you think you might have IT Band Syndrome, it is important to see a doctor or physical therapist who can help you develop a plan to manage your symptoms and prevent future problems.
Diagnostic Ultrasound:
Diagnostic ultrasound is very helpful for assessment of iliotibial band friction syndrome. As this is a dynamic modality we we will be able to see the IT band as it moves over the lateral epicondyle of the knee during extension and flexion of the knee. This allows us to evaluate for any thickening of the ITB but also to identify any iliotibial bursitis which is indicated by fluid in the iliotibial bursa.
 In addition to the clinical findings ultrasound can also be helpful in ruling out other potential sources of lateral knee pain such as ligamentous injuries or meniscal tears.
In addition to the clinical findings ultrasound can also be helpful in ruling out other potential sources of lateral knee pain such as ligamentous injuries or meniscal tears.
The ultrasound-guided injection procedure allows very specific targeting of the iliotibial bursa. The bursa is clearly identifiable on ultrasound and for a skilled practitioner the needle is then accurately guided in the ITB bursa which lies superficial of the lateral femoral condyle and underneath the iliotibial band. The accurate administration of steroid also avoids potential weakening of the IT band by inadvertent injection in the body of the IT band which is very realistic possibility if this injection is done unguided.
Conclusion:
ITB friction syndrome is a frequent overuse injury which often affects runners but also cyclists. This is a condition that can lead to significant pain and loss of function making it difficult if not impossible to exercise. Initial management is with non-invasive options such as physiotherapy treatment rest, stretches, strengthening exercises and nonsteroidal anti-inflammatory drugs. If these options are not sufficient then ultrasound-guided steroid injection is a very effective option to quickly reduce inflammation and thus reduce pain.
Diagnostic ultrasound is very helpful in accurately diagnosing the condition and then also allowing accurate injection of a steroid in the inflamed bursa between IT band and lateral femoral condyle
In the Sonoscope clinic we provide a One-Stop-Clinic which includes clinical diagnosis, diagnostic ultrasound and ultrasound-guided injection all within the One session.
Guidelines for Frequency of Steroid Injections
Steroid injections are generally used to reduce inflammation and pain.
We will look at the guidance on the frequency of these injections. There is some evidence from studies on people with rheumatoid arthritis suggesting that multiple steroid injections in the same joint are safe to administer (1). However, injection therapy frequency must be seen in the context of the individual patient. In very young patients, repeat injections are avoided, if possible, given their young age and the possibility that more injections could be required, and only a finite number of repeat injections can be given.
However, there may not be any other treatment options available for elderly patients, such as those with severe pain and/or dysfunction, especially if a previous steroid injection has been administered and was successful for a long time.
There are limitations to the maximum frequency of steroid injections that can be given. It is generally accepted that no more than 3 steroid injections in any one joint should be given per year.
Again, context is everything here. I think that many practitioners would hesitate to do 3 injections/year every year in perpetuity. And again, in young people, most would agree that it is inappropriate to continue with repeat steroid injections x 3 in the same joint year after year. Even in older patients, most practitioners would also be quite careful, but if no other options exist and the patient does get very good pain relief, then in some instances, more than 3 in total might be given.
Another factor to consider is the amount of time between injections that should be allowed before a repeat steroid injection can be administered. NHS guidelines https://www.nhs.uk/conditions/steroid-injections/ suggest that there should be a 3-month gap between steroid injections, although context is everything here and in specific cases, a steroid injection given after 6 weeks might be acceptable.
Side-effects: It is well-known that long-term, excessive use of steroid injections can lead to significant structural damage such as: Thinning of the soft tissue and skin and muscle tissue, weakening of cartilage and bone, increase the risk of joint infection and possible increased glucose levels leading to diabetes. Please also see this link to a post on the side effects of steroid injections.
- Combe B. Early rheumatoid arthritis: strategies for prevention and management. Best Pract Res Clin Rheumatol. 2007;21: 27-42.
The Role of Steroid Injections in Treating Arthritis
Steroid Injections in Treating Arthritis
Steroid injections are commonly used in musculoskeletal conditions such as osteoarthritis. However, they can also play an important role in managing joints affected by inflammatory arthritis such as Rheumatoid arthritis or psoriatic arthritis or conditions such as gout.
Through complex processes, steroids have powerful anti-inflammatory effects, which help to reduce the levels of inflammation of the joint in question. Pain levels will improve with the reduction in inflammation. The mechanism of action leads to a decrease in synovial blood flow and the number of leukocytes, as well as the release of inflammatory mediator (1). Joint inflammation in knee OA is associated with progression of cartilage damage, therefore steroid injection might reduce disease progression.
As indicated above, inflammation causes swelling and pain. Steroid injections, therefore, can reduce swelling of joints and other structures affected by inflammation. This will help with mobility and function.
It is well-known that steroid injections have a temporary effect, but this can last for a good number of months. It is therefore not uncommon that for those with self-limiting conditions such as: Frozen shoulder, certain degrees of tendinopathy and bursitis etc. a single steroid injection might be sufficient for the problem to disappear completely and for it to never return. The reason for this is that natural healing will take place, and by the time that the steroid has stopped working the person has recovered naturally.
Of course, for more chronic conditions with significant structural damage, such as significant degrees of osteoarthritis, the benefit of the steroid injection is often more temporary in nature although from experience I have found that in a good number of cases the steroid helps to settle the acute pain for months at which point the joint might have settled naturally in a state where pain is no longer a significant issue despite the fact that the degenerative changes present are still unchanged.
In the case of osteoarthritis if someone does require repeat injections, they may well benefit from hyaluronic acid injections, which contain hyaluronic acid (a natural component of joint fluid). These injections contain a synthetic form of hyaluronic acid and help to lubricate the affected joint.
Rastogi, A.K.; Davis, K.W.; Ross, A.; Rosas, H.G. Fundamentals of Joint Injection. Am. J. Roentgenol. 2016, 207, 484–494.
Steroid or hyaluronic acid injection for osteoarthritis of the Knee
Both steroid as well as hyaluronic acid are commonly used in the treatment of osteoarthritis of the knee.
Steroid injections work through complex processes, and they have powerful anti-inflammatory effects, which help to reduce the levels of inflammation of the joint in question. Pain levels will improve with the reduction in inflammation. Steroid injections can provide very quick relief, usually within days, and can last for many months. Steroid injection can be repeated this has to be done with care as you take too many repeat injections can cause damage to the tissues within the knee joint (cartilage).
Hyaluronic acid injections help to lubricate the joint. Hyaluronic acid injections are replicating the natural fluid that occurs in the knee joint. The length of time the people can benefit from these injections is variable and can range from a month to 6 months or so. The success is dependent on many factors including the degree of structural damage to needed degree of active inflammation of the knee et cetera.
Altman et al. (2015) did a systematic review into the mechanisms of action of hyaluronic acid injections for osteoarthritic knees (Altman, R.D., Manjoo, A., Fierlinger, A., Niazi, F. and Nicholls, M., 2015. The mechanism of action for hyaluronic acid treatment in the osteoarthritic knee: a systematic review. BMC musculoskeletal disorders, 16, pp.1-10.)
Key mechanisms of action reported:
- Chondroprotection (protection of cartilage) was mentioned by 64.42 % of the articles used in the study. 67 of the studies included described Chondro protective effects of intra-articular hyaluronic acid treatment. Intra-articular hyaluronic acid has been shown to reduce chondrocyte apoptosis, while increasing chondrocyte proliferation.
- Proteoglycan/Glycosaminoglycan synthesis was mentioned by 21.15 % and in 22 of the studies involved who mentioned the enhanced proteoglycan and glucosamine glycan synthesis related to intra-articular hyaluronic acid treatment. As osteoarthritis progresses intrinsic proteoglycan and GAG concentrations decline within the cartilage. Results demonstrated that intra-articular hyaluronic acid treatment stimulated proteoglycan synthesis delaying the progression of osteoarthritis.
- Anti-inflammatory effects were mentioned by 20.19 % in 21 of the identified studies the anti-inflammatory effects of intra-articular hyaluronic acid treatment was mentioned. IL-1β is known to demonstrate pro inflammatory effects and suppression of IL-1β by hyaluronic acid provides anti-inflammatory effects.
- Mechanical effects were mentioned by 9.61 % or 10 of the studies that were included describe mechanical effects of hyaluronic acid in the treatment of osteoarthritis of the knee. Fiscus nature of hyaluronic acid treatment is shown to lubricate joint capsule preventing degeneration through decreased flexion. Hyaluronic acid further protects the joint capsule through beneficial shock absorption effects. Hyaluronic acid provides cushioning to absorb pressure and vibration within the joint that otherwise would lead to chondrocyte degeneration.
- Subchondral Bone was mentioned by 7.69 % Or 8 of the included studies. He has been shown that interaction between subchondral bone osteoblast and articular cartilage is chondrocytes in osteoarthritic joints alters. Several enzymes play a role in collagen degradation as well as cartilage degradation. Intra-articular hyaluronic acid affects the subchondral bone mainly by suppression of these enzymes.
- Analgesic was mentioned by 5.76 % or 6 of the included articles described significant decrease in pain associated behaviour with a single hyaluronic acid injection in a murine model. One of the studies suggested that hyaluronic did not directly bind to bradykinin receptors but provided analgesic effects through interactions with hyaluronic acid in the receptors and free nerve endings within the joint tissue.
Steroid Injections
Steroid injections are often used due to their fast course of action
Through complex processes, steroids have powerful anti-inflammatory effects, which help to reduce the levels of inflammation of the joint in question. In most cases accurately administered steroid injections can provide pain relief often within 24 to 48 hours. Joint mobility can rapidly improve due to reduction of inflammation and pain which in turn helps function. Steroid injections due to being administrated locally have fewer side effects then oral steroids.
Known side effects of steroid injections: Depigmentation of skin post injection, repeated steroid injections can cause cartilage damage. Steroid injections can weaken tendons and increase the risk of tendon rupture in some cases. People may experience facial flushing which usually last for a few hours. There is also very rare possibility of an infection following a steroid injection which is uncommon and thought to be in the order of 4.6 per 100,000 injections.
Other injection related risks are neurovascular injury which can occur with any injection and is not specifically related to steroid injection
Conclusion: Which is better: Steroid or Hyaluronic acid injection?
Both steroid and hyaluronic acid injections are commonly used to treat osteoarthritis of the knee, but they work in different ways and have distinct benefits and drawbacks.
I would generally recommend steroid injections in scenarios where there is a very high level of pain making function difficult. Often there is then also a significant degree of inflammation present in many cases with effusion and neovascularity on ultrasound. In those cases, and of course if there is no contraindication, I would favour steroid injection. As this tends to act rapidly with significant pain relief which can be sustained for many months.
If levels of function are slightly better and pain levels are more modest and structural changes to the joint are mild to moderate, then hyaluronic acid injection can be a very good option.
One very important thing to remember is that steroid injections come with potential side effects as listed above and those side effects tend to become more frequent the more often steroid injections are given in the same structure. Hyaluronic acid injections do not have this drawback and can be repeated if successful an infinite number of times.
References:
Altman, R.D., Manjoo, A., Fierlinger, A., Niazi, F. and Nicholls, M., 2015. The mechanism of action for hyaluronic acid treatment in the osteoarthritic knee: a systematic review. BMC musculoskeletal disorders, 16, pp.1-10.
Bilsborough Smith, C., Baker, D., Botchu, R., Cairns, M., Chester, R., Dean, B., Mast, R. and Lewis, J., 2023. Corticosteroid injections for non-spinal musculoskeletal conditions. Consideration of local and systemic adverse drug reactions and side effects. New Zealand Journal of Physiotherapy.
Holland, C., Jaeger, L., Smentkowski, U., Weber, B. and Otto, C., 2012. Septic and aseptic complications of corticosteroid injections: an assessment of 278 cases reviewed by expert commissions and mediation boards from 2005 to 2009. Deutsches Ärzteblatt International, 109(24), p.425.
How long does an ultrasound-guided injection last for?
How long does an ultrasound-guided injection last for?
Accuracy of diagnosis:
This really depends on several factors. First, it depends on an Accurate Diagnosis of the problem. For example if someone has been incorrectly diagnosed with a frozen shoulder whilst their problem is related to a rotator cuff tear then injecting the incorrect structure i.e: shoulder joint with a steroid is unlikely to result in significant pain relief.
Ultrasound guided injections are more effective and efficacious then unguided injections
There is significant evidence that ultrasound guided injections are more accurate than unguided injections via systematic review and meta-analysis by Hoeber et al: 2016. A Systematic review by Aly et al. (2015) also showed that shoulder girdle injections are also more effective.
Type of injection given:
Steroid injections are generally thought to be lasting a good number of months although of course many conditions will naturally improve within that timeframe anyway so a good number of people will remain symptom-free following the injection. For conditions where there is significant structural damage such as degenerative changes of joints or significant tendon defects the benefit of a steroid injection is likely to be of a temporary nature. Generally speaking in these scenarios I would expect it to perhaps last for 3 to 4 months. Every condition however is different and people with very severe degenerative changes for example might actually not have much benefit at all from a steroid injection. Although we cannot be sure about this as we all know people with exactly the same condition who will get real good benefit for many months.
Hyaluronic acid injections are thought to be longer lasting and oftentimes people have benefits for 6 months or longer still. Usually, hyaluronic acid injections are less beneficial for those with more severe degenerative changes. If the person to be injected has mild to perhaps moderate changes they might have a better outcome.
Arthrosamid Injections studies have shown that Arthrosamid can give people long lasting pain relief. Studies have indicated that 1 injection can be enough to give people 3 years of significant pain relief.
In Summary:
If done under ultrasound guidance injections are more accurate and therefore can give better pain relief and for longer. Steroid injections tend to last for a good number of months, hyaluronic acid injections can last for longer possibly 6 months to maximum a year. Arthrosamid injections can give significant pain relief for people with knee arthritis for up to 3 years.
References:
Aly AR, Rajasekaran S, Ashworth N. Ultrasound-guided shoulder girdle injections are more accurate and more effective than landmark-guided injections: a systematic review and meta-analysis. British journal of sports medicine. 2015 Aug 1;49(16):1042-9.
Hoeber, S., Aly, A.R., Ashworth, N. and Rajasekaran, S., 2016. Ultrasound-guided hip joint injections are more accurate than landmark-guided injections: a systematic review and meta-analysis. British Journal of Sports Medicine, 50(7), pp.392-396.
Looking for an expertly delivered and pinpoint accurate injection?
You are in the right place!
With thousands of successful ultrasound guided injections behind him contact our lead clinician Rob Mast for a free telephone consulation.
We are proud to bring our highly specialist ultrasound guided procedures to a physiotherapy practice in your local area !
Check out our competetive fees!
Cubital Tunnel Injection: An effective way to relief pain from cubital tunnel syndrome
Cubital tunnel syndrome can be a painful and debilitating condition. It affects the ulnar nerve, which runs through the elbow, causing numbness, tingling, and pain in the arm and hand. For those suffering from this syndrome, finding effective treatment is crucial to regain their quality of life.
Sonoscope provides pinpoint accurate injections paving the way for enduring comfort and enhanced mobility. Cubital tunnel syndrome can significantly affect everyday tasks and overall well-being, underscoring the importance of effective treatment.
This detailed guide will cover everything you need to know about Cubital tunnel syndrome and pain relief.
Why Is It Important To Understand Cubital Tunnel Syndrome?
Understanding cubital tunnel syndrome is very important because it helps people know what to do if they have symptoms. Cubital tunnel syndrome happens when the ulnar nerve in your elbow gets squeezed or irritated. This nerve runs from your neck down to your hand. It can cause problems like numbness, tingling, or pain in your ring and little fingers, and even make your hand feel weak. Knowing about this condition can help you recognize these symptoms early and get the right treatment before it gets worse.
One reason it is important to understand cubital tunnel syndrome is that it can really affect your daily life. Imagine trying to do your homework, play your favorite video games, or even eat with chopsticks when your hand is numb or hurts. It would make everything harder and less fun. If you know what to look for, you can tell an adult, like your parents or a teacher, so they can help you get to a doctor. The clinician can figure out if you have cubital tunnel syndrome and what you need to do to feel better.
Another reason to understand cubital tunnel syndrome is that early treatment can prevent more serious problems. If the nerve stays squeezed for too long, it can get damaged. This can make it even harder to use your hand. Doctors might suggest different treatments, like wearing a splint to keep your elbow straight, doing special exercises, or in some cases, having surgery. The sooner you start treatment, the better your chances of avoiding long-term problems.
Knowing about cubital tunnel syndrome can also help you avoid things that make it worse. For example, if you spend a lot of time leaning on your elbows, like when you are reading a book or using your computer, it can put extra pressure on the nerve. By understanding this, you can learn to change your habits to protect your elbow. You might take breaks more often, use a pillow to rest your elbows on, or try to sit in a way that doesn’t put pressure on your elbows. These small changes can make a big difference in keeping the nerve healthy.
Hence, understanding this condition is important for everyone, not just adults. Kids can get cubital tunnel syndrome too, especially if they do activities that put a lot of stress on their elbows. By learning about it now, you can take steps to keep your elbows safe and avoid problems in the future.
What Are The Benefits Of Sonoscope For Cubital Tunnel Syndrome?
Cubital tunnel syndrome is a condition that happens when the ulnar nerve in your elbow gets squeezed or pressed. This can make your hand and fingers feel numb or tingly, and it can even make your muscles weak. If you have this problem, doing simple things like holding a cup or opening a jar can become very hard.
Some common treatments include physical therapy, medications, and sometimes surgery. However, there’s a new and exciting treatment called Sonoscope that can help with cubital tunnel syndrome.
At Sonoscope we pride ourselvesin giving very accurate injections. injections are done ultrasound guided, This means the clinician can see exactly where the needle is going and make sure it goes to the right spot. This is very important because it helps the medicine go exactly where it is needed, which makes the treatment work better.
Because the clinican can see exactly where the needle is going, it makes sure that the injection is very accurate. It also means there is less risk of damaging other parts of your body, like muscles or blood vessels, during the injection.
Another great thing about Ultrasound guided injections is that they are minimally invasive. This means that it doesn’t involve big cuts or a lot of recovery time. Surgery can be very painful and take a long time to heal, but ultrasound guided njections are much simpler. They are done with a small needle, so the procedure is quick, and you can go home the same day. This also means you can get back to your normal activities faster.
People who have used Sonoscope to treat their cubital tunnel problems have reported very good results. Patients have said they feel less pain and their hand and finger movements improve. This means they can do everyday tasks more easily. Some patients have even said that the treatment helped them avoid surgery, which can be a big relief.
Many patients who have tried Sonoscope are happy with the results. They say the treatment is not very painful and that it helps them feel better quickly. The treatment is also very convenient because it doesn’t take a lot of time, and you don’t have to stay in the hospital.
Conclusion
Sonoscope’s cubital tunnel injection offers a revolutionary treatment for those suffering from cubital tunnel syndrome. It has a non-invasive nature, quick recovery time, and long-lasting relief make it an excellent alternative to traditional treatments. By choosing ultrasound guided injections provided by Sonoscope, patients can look forward to improved quality of life and effective management of their symptoms. If you or someone you know is struggling with cubital tunnel syndrome, consider contacting Sonoscope Ltd.