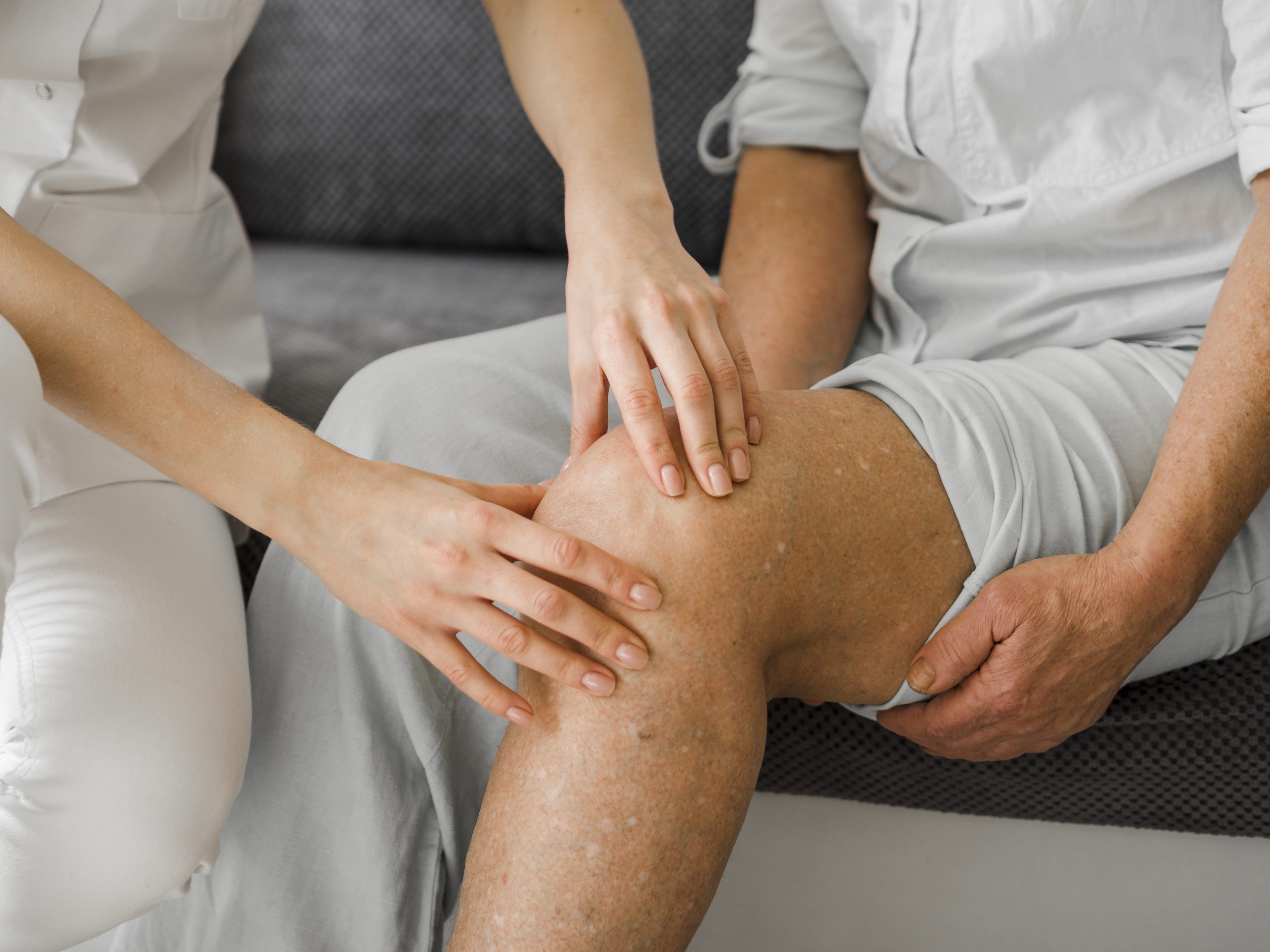
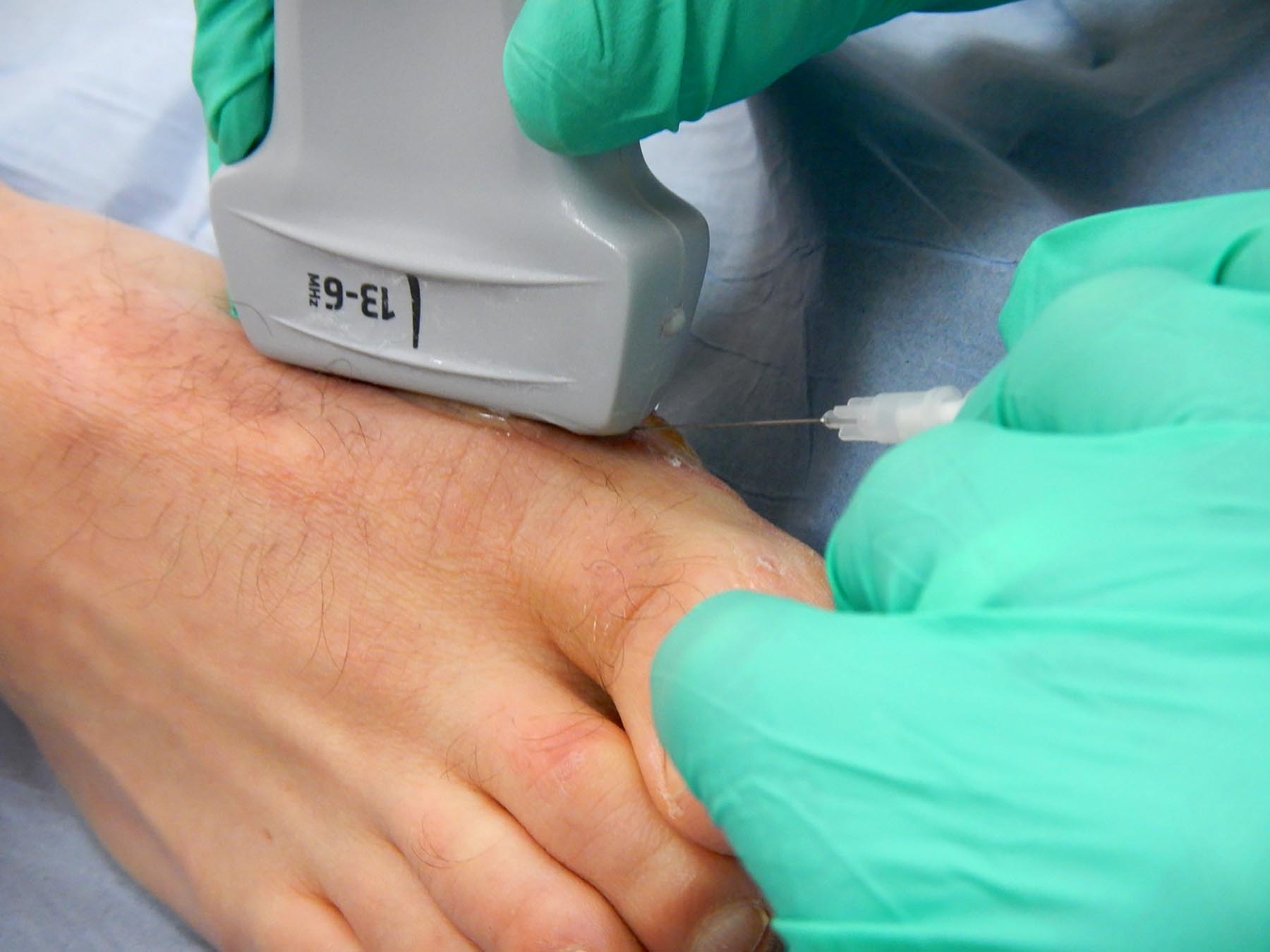
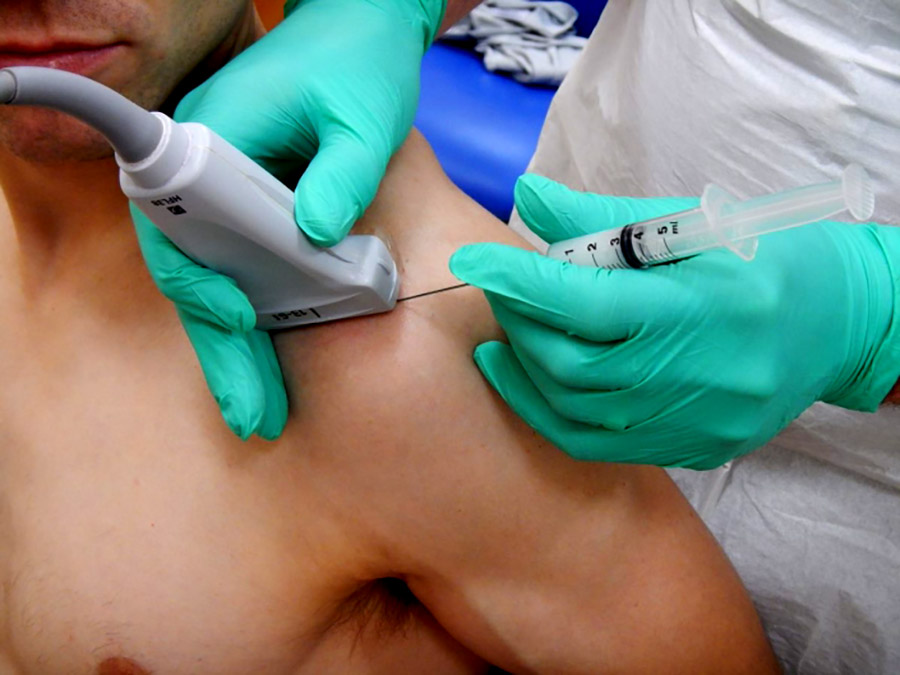
Steroid or hyaluronic acid injection for osteoarthritis of the Knee
Both steroid as well as hyaluronic acid are commonly used in the treatment of osteoarthritis of the knee.
Steroid injections work through complex processes, and they have powerful anti-inflammatory effects, which help to reduce the levels of inflammation of the joint in question. Pain levels will improve with the reduction in inflammation. Steroid injections can provide very quick relief, usually within days, and can last for many months. Steroid injection can be repeated this has to be done with care as you take too many repeat injections can cause damage to the tissues within the knee joint (cartilage).
Hyaluronic acid injections help to lubricate the joint. Hyaluronic acid injections are replicating the natural fluid that occurs in the knee joint. The length of time the people can benefit from these injections is variable and can range from a month to 6 months or so. The success is dependent on many factors including the degree of structural damage to needed degree of active inflammation of the knee et cetera.
Altman et al. (2015) did a systematic review into the mechanisms of action of hyaluronic acid injections for osteoarthritic knees (Altman, R.D., Manjoo, A., Fierlinger, A., Niazi, F. and Nicholls, M., 2015. The mechanism of action for hyaluronic acid treatment in the osteoarthritic knee: a systematic review. BMC musculoskeletal disorders, 16, pp.1-10.)
Key mechanisms of action reported:
- Chondroprotection (protection of cartilage) was mentioned by 64.42 % of the articles used in the study. 67 of the studies included described Chondro protective effects of intra-articular hyaluronic acid treatment. Intra-articular hyaluronic acid has been shown to reduce chondrocyte apoptosis, while increasing chondrocyte proliferation.
- Proteoglycan/Glycosaminoglycan synthesis was mentioned by 21.15 % and in 22 of the studies involved who mentioned the enhanced proteoglycan and glucosamine glycan synthesis related to intra-articular hyaluronic acid treatment. As osteoarthritis progresses intrinsic proteoglycan and GAG concentrations decline within the cartilage. Results demonstrated that intra-articular hyaluronic acid treatment stimulated proteoglycan synthesis delaying the progression of osteoarthritis.
- Anti-inflammatory effects were mentioned by 20.19 % in 21 of the identified studies the anti-inflammatory effects of intra-articular hyaluronic acid treatment was mentioned. IL-1β is known to demonstrate pro inflammatory effects and suppression of IL-1β by hyaluronic acid provides anti-inflammatory effects.
- Mechanical effects were mentioned by 9.61 % or 10 of the studies that were included describe mechanical effects of hyaluronic acid in the treatment of osteoarthritis of the knee. Fiscus nature of hyaluronic acid treatment is shown to lubricate joint capsule preventing degeneration through decreased flexion. Hyaluronic acid further protects the joint capsule through beneficial shock absorption effects. Hyaluronic acid provides cushioning to absorb pressure and vibration within the joint that otherwise would lead to chondrocyte degeneration.
- Subchondral Bone was mentioned by 7.69 % Or 8 of the included studies. He has been shown that interaction between subchondral bone osteoblast and articular cartilage is chondrocytes in osteoarthritic joints alters. Several enzymes play a role in collagen degradation as well as cartilage degradation. Intra-articular hyaluronic acid affects the subchondral bone mainly by suppression of these enzymes.
- Analgesic was mentioned by 5.76 % or 6 of the included articles described significant decrease in pain associated behaviour with a single hyaluronic acid injection in a murine model. One of the studies suggested that hyaluronic did not directly bind to bradykinin receptors but provided analgesic effects through interactions with hyaluronic acid in the receptors and free nerve endings within the joint tissue.
Steroid Injections
Steroid injections are often used due to their fast course of action
Through complex processes, steroids have powerful anti-inflammatory effects, which help to reduce the levels of inflammation of the joint in question. In most cases accurately administered steroid injections can provide pain relief often within 24 to 48 hours. Joint mobility can rapidly improve due to reduction of inflammation and pain which in turn helps function. Steroid injections due to being administrated locally have fewer side effects then oral steroids.
Known side effects of steroid injections: Depigmentation of skin post injection, repeated steroid injections can cause cartilage damage. Steroid injections can weaken tendons and increase the risk of tendon rupture in some cases. People may experience facial flushing which usually last for a few hours. There is also very rare possibility of an infection following a steroid injection which is uncommon and thought to be in the order of 4.6 per 100,000 injections.
Other injection related risks are neurovascular injury which can occur with any injection and is not specifically related to steroid injection
Conclusion: Which is better: Steroid or Hyaluronic acid injection?
Both steroid and hyaluronic acid injections are commonly used to treat osteoarthritis of the knee, but they work in different ways and have distinct benefits and drawbacks.
I would generally recommend steroid injections in scenarios where there is a very high level of pain making function difficult. Often there is then also a significant degree of inflammation present in many cases with effusion and neovascularity on ultrasound. In those cases, and of course if there is no contraindication, I would favour steroid injection. As this tends to act rapidly with significant pain relief which can be sustained for many months.
If levels of function are slightly better and pain levels are more modest and structural changes to the joint are mild to moderate, then hyaluronic acid injection can be a very good option.
One very important thing to remember is that steroid injections come with potential side effects as listed above and those side effects tend to become more frequent the more often steroid injections are given in the same structure. Hyaluronic acid injections do not have this drawback and can be repeated if successful an infinite number of times.
References:
Altman, R.D., Manjoo, A., Fierlinger, A., Niazi, F. and Nicholls, M., 2015. The mechanism of action for hyaluronic acid treatment in the osteoarthritic knee: a systematic review. BMC musculoskeletal disorders, 16, pp.1-10.
Bilsborough Smith, C., Baker, D., Botchu, R., Cairns, M., Chester, R., Dean, B., Mast, R. and Lewis, J., 2023. Corticosteroid injections for non-spinal musculoskeletal conditions. Consideration of local and systemic adverse drug reactions and side effects. New Zealand Journal of Physiotherapy.
Holland, C., Jaeger, L., Smentkowski, U., Weber, B. and Otto, C., 2012. Septic and aseptic complications of corticosteroid injections: an assessment of 278 cases reviewed by expert commissions and mediation boards from 2005 to 2009. Deutsches Ärzteblatt International, 109(24), p.425.
What is physiotherapy?
What is physiotherapy?
Physiotherapy as described by World Physiotherapy is a health care profession concerned with human function and movement and maximising physical potential. It is concerned with identifying and maximising quality of life and movement potential within the spheres of promotion, prevention, treatment/intervention, habilitation and rehabilitation[1]. It uses physical approaches to promote, maintain and restore physical, psychological and social well-being, taking into account variations in health status. It is science-based, committed to extending, applying, evaluating and reviewing the evidence that underpins and informs its practice and delivery. The exercise of clinical judgement and informed interpretation is at its core[2].
What do physiotherapists do?
Physiotherapy is a healthcare profession that provides services to people of all ages, from newborns to the elderly. Physiotherapists help people who are recovering from an injury or illness, or who have a long-term health condition, such as arthritis.
Physiotherapists work in hospitals, clinics, community health centres, private practices and people’s homes. They may also work in industrial and sporting settings.
Physiotherapy addresses the illnesses or injuries that limit a person’s abilities to move and perform functional activities in their daily lives.[7] Physiotherpists take an individual’s history and physical examination to arrive at a diagnosis and establish a management plan and, when necessary, incorporate the results of laboratory and imaging studies like X-rays, CT-scan, or MRI findings. Electrodiagnostic testing (e.g., electromyograms and nerve conduction velocity testing) may also be used.[8]
What are the benefits of physiotherapy?
Physiotherapy can benefit people of all ages. It helps to restore movement and function when someone is affected by injury, illness or disability.
Physiotherapy can:
- Alleviate pain
- Increase mobility
- Improve quality of life
How can physiotherapy help me?
Physiotherapy is a branch of medicine that deals with the assessment, diagnosis, and treatment of physical and functional impairments. Physiotherapy can help you by improving your mobility, relieving pain, and preventing or managing injuries.
What conditions can physiotherapy help?
Physiotherapy can help a range of conditions, from everyday aches and pains, to more complex long-term conditions. It can also help you prevent injuries from happening in the first place.
Some of the conditions physiotherapy can help with are:
-joint and muscle pain, including back pain and neck pain
-arthritis
-frozen shoulder
-tendonitis
-sprains and strains
-whiplash
-headaches caused by muscle tension
How does physiotherapy help?
Physiotherapy is a health care profession that provides services to individuals and populations to develop, maintain and restore maximum movement, function and wellbeing throughout the lifespan. It involves the assessment, diagnosis, treatment and prevention of musculoskeletal, neurological, cardiovascular and respiratory conditions.
What can I expect from physiotherapy?
Physiotherapy is a rehabilitation profession that uses a range of techniques to alleviate pain, promote movement and restore function. The aim of physiotherapy is to help you live your life to the fullest potential.
What will happen during my first visit?
At your first visit, the physiotherapist will take a thorough medical history and perform a physical examination. They may also order tests, including X-rays, MRIs, and blood tests. The physiotherapist will use this information to develop a treatment plan specifically for you.
How often will I need to see a physiotherapist?
This will depend on the severity and nature of your injury or condition. In some cases, you may only need to see a physiotherapist once or twice. In other cases, you may need to see a physiotherapist on a regular basis for several months.
How can I find a physiotherapist?
To practise as a physiotherapist in the UK you must be registered with the Health and Care Professions Council (HCPC), which is the regulatory body for physiotherapists and some other allied health professions (AHPs).
Your GP might refer you via the NHS to see a physiotherapist. Privately you might find a physiotherapist through recommendation or via an internet search for local physiotherapists. Please make sure that you find out if your physiotherapist is fully trained and competent by checking their status on the HCPC register check here
To become registered with the HCPC as a physiotherapist you must meet the HCPC criteria. Physiotherapists need to meet three sets of standards (please see click the links to see each set of standards): Standards of conduct, performance and ethics, Standards of proficiency for physiotherapists, Standards of continuing professional development.
Physiotherapists also need to have professional liability insurance (PLI) in order to be registered with the HCPC.
How do I know if a physiotherapist is right for me?
Before you book an appointment with a physiotherapist, it’s important to do your research to make sure they’re the right fit for you.
A good place to start is by asking for recommendations from friends, family, or your primary care doctor. Once you have a few names, you can check their credentials (please see above re professional registration)
You can also look up reviews online, or contact the physiotherapist directly to ask about their experience and treatment methods. When you meet with them, be sure to ask plenty of questions so that you feel comfortable with their approach.
Once you’ve found a physiotherapist that you trust, they will be able to assess your condition and develop a treatment plan that is tailored to your needs.
What should I look for in a physiotherapist?
There are many things to consider when looking for a physiotherapist. Below are some factors you may want to keep in mind:
- What is the physiotherapist’s education and training?
- How long has the physiotherapist been in practice?
- Is the physiotherapist registered with the HCPC?
- What is the physiotherapist’s approach to treatment?
- Does the physiotherapist have experience treating patients with conditions similar to yours?
- Does the physiotherapist use modalities that you are comfortable with?
- Is the physiotherapist’s office conveniently located and easy to get to?
- Is the staff friendly and helpful?
- Do you feel comfortable communicating with the physiotherapist?
What if regular physiotherapy is unable to help me?
If physiotherapy alone isn’t enough to improve your problem then seeing an advanced practice physiotherapist can be helpful. Usually regular physiotherapists either work with or are aware of specialist physiotherapists with an extended skill set. They are usually referred to as Advanced PracticePphysiotherapists (APPs).
Often times in musculoskeletal physiotherapy they have added skills and competencies. So they may be trained as: Injection therapists, sonographers, or prescribers of medicines. A highly trained Advanced Practice Physiotherapist might be able to help where regular physiotherapy has stalled and where diagnostic imaging is required as well as potential injection therapy to manage the problem.
Advanced Practice Physiotherapy
Robert Mast who is the owner and clinical director of Sonoscope ultrasound guided injections he is a highly trained Advanced Practice Physiotherapist (APP) and is a (CASE accredited) qualified expert in diagnostic ultrasound as well as an independent prescriber of medicines and an experienced injector. He has worked in the NHS for many years in specialist MSK services managing complex musculoskeletal conditions. He is also employed as a specialist MSK sonographer in a busy NHS radiology performing many diagnostic ultrasound scans and ultrasound guided interventions for those with musculoskeletal injuries and conditions . He is also an experienced educator and runs university based (Brunel University) diagnostic ultrasound as well as ultrasound guided injections programs. Please click Robert Mast to get in touch with and he will get back to you as soon as possible.
Secondary care specialists
In certain scenarios medical input is required.
For example: an Orthopaedic consultant is needed when Orthopaedic surgery is considered maybe to repair a bone, ligament of tendon or to replace a joint (for example a hip or knee joint). In case of an inflammatory arthitis is suspected then referral to a rheumatologist would be required. In case of a neurological problem a neurologist opinion might be necessary etc.
What is Advanced Practice Physiotherapy?
What is Advanced Practice Physiotherapy?
Advanced practice (AP) enables physiotherapists to incorporate advanced level skills and knowledge within their physiotherapy practice.
These Advanced Practice Physiotherapists (APPs) use their skills to address complex decision-making processes in the management
of patients with a range of presentations in both intervention and preventive care. APPs have completed an advanced programme of
studies beyond their initial physiotherapy training which will include the development of a range of skills and knowledge such as for example independent
prescribing.
What does this mean in practice?
- The advanced practice physio will use a combination of advanced skills, knowledge and attitudes which enables him to address complex problems and manage risk in unpredictable contexts
- The advanced practice physiotherapist will us advanced critical thinking todeliver care to patients with complex needs safely and competently.
- The advanced practice physiotherapist has the ability to recognise and manage unfamiliar presentations, recognising where a clinical presentation
is outside an individual’s scope and take appropriate action.
What can I expect from Sonoscope?
At Sonoscope we are committed to provide the highest level of care for our patients. To deliver the One-Stop-Clinic experience the levels of skills required by the practioner have to be of the highest level of advanced practice physiotherapy
Robert Mast who is the owner and clinical director of Sonoscope ultrasound guided injections is a a highly trained and (CASE accredited) qualified expert in diagnostic ultrasound as well as an independent prescriber of medicines and an experienced injector. He has worked in the NHS for many years in specialist MSK services managing complex musculoskeletal conditions. He is also employed as a specialist MSK sonographer in a busy NHS radiology department performing many diagnostic ultrasound scans and ultrasound guided interventions for those with musculoskeletal injuries and conditions. In addition to that he is an experienced educator and runs university based (Brunel University) diagnostic ultrasound as well as ultrasound guided injections programs.
You can rest assured that the care provided is the complete integrated package .
- You will receive a clinical assessment (taking the history and carrying out an expert physical assessment)
- You will then have a diagnostic ultrasound scan
- If indicated you may then also have an ultrasound guided injection
This will all be done within the one session
Steroid injection for shoulder bursitis
Steroid Injection for shoulder bursitis
What is shoulder bursitis?
Bursae (plural) are potential fluid-filled sacs that are part of the skeletal system. They cushion the space between bones and connective tissue, allowing tendons, muscle and bone to move together.
In the shoulder, the subacromial bursae cushion the area between the rotator cuff tendons and the acromion (the highest point of the shoulder blade or scapula). Bursae allow the tendons and bones to glide without friction when you move and lift your arms.
Injuries or overuse of the shoulder can cause swelling of the bursae. Often the term subacromial bursitis is used to refer to bursitis that affects the shoulder.
Symptoms:
You may have bursitis if a part of your body, particularly areas close to a joint or directly over a bone, is red or swollen, hot and sore, painful – usually with a dull, aching pain . The area is sensitive and painful if you try to press on or move it, If the bursa is just under your skin, you may also be able to see its outline, because of the swelling inside it.
Are there different types of bursitis?
Chronic:
Injuries or repetitive activities can lead to irritation of the subacromial bursa causing shoulder bursitis. Significant structural injuries such as damaged tendons or irregular or damaged bone may also contribute to irritation of the subacromial bursa leading to recurrent/chronic bursitis.
Acute:
This is usually a bursitis of a sudden onset often due to a trauma
Septic:
In very unusual and rare cases bursa can become infected which can be related to a skin piercing injury. Usually, the shoulder feels hot and swollen as well as red the pain can be severe
Common locations of bursitis:
The most common locations for bursitis are in the shoulder, elbow and hip. However, it can also occur in the knee, heel and the base of the big toe. Bursitis often occurs near joints that perform frequent repetitive motion.
Causes:
Bursitis is caused by inflammation of small fluid pads that overlie areas of strain and stress such as tendons and bones. The normal situation the small pads actually help to make normal movements run very smooth and without any pain and discomfort. However when they become inflamed sometimes due to increased irritation and local stress on the body part they can swell up and become very painful and causing significant impact on normal function.
How would you know if you have a bursitis?
When as mentioned above you have inflammation of the bursa the bursa might be swollen and painful. This can have a significant impact on the movement of the body part. Pain from the bursitis is usually a dull ache. It can be significantly red and swollen as well.
Some inflammatory conditions such as rheumatoid arthritis can cause bursitis and another inflammatory conditions such as gout can cause crystals in or around the joints that can cause bursitis as well.
Often the area where there is strain on tendons such as around the knee the shoulder or the hip can result in bursitis. The underlying source here is usually a tendon which might need treatment which can improve the bursitis.
What treatment can be helpful?
If the pain is quite acute than ice packs on the affected area can be very helpful. Cushioning of the affected area can be helpful. This can be her a foam pad for example or a specific support with padding.
Physiotherapy can be helpful in particular to address the underlying issues causing the bursitis. Specific exercises and conditioning can help to improve tendon function and reduce bursitis as a result.
Medication can in some cases be helpful. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) can be helpful to reduce the most acute pain
What to do if the symptoms do not improve?
If you have a temperature then do see your GP. If the skin overlying the bursa has been broken then also see your GP.
If symptoms do not improve but do not have the features as mentioned above (signs of infection) then assessment by a practitioner with specialist musculoskeletal assessment skills would help to diagnose the problem. Examination of the body part should identify the exact problem. A further ultrasound scan would confirm the findings. Sometimes aspiration of the fluid is necessary usually with steroid injection to bring down the local inflammation.
A One-Stop clinic to both diagnose and treat bursitis:
The fastest and most effective way to manage this problem if the above management strategies have not been effective would be to be seen in a one-stop clinic.
The Sonoscope diagnostic ultrasound and ultrasound guided injection clinic offers an expert assessment of the body part involved. Diagnostic ultrasound then follows to confirm the diagnosis and following that and after discussion and if appropriate potentially a steroid injection and/or aspiration can be carried out. This would all be done within the one session without the need for any wait and without the need for any extra expenses.
Diagnostic ultrasound and ultrasound guided injections
When clinical examination reveals that this is a bursitis then ultrasound can help to confirm it and ultrasound will also allow an appropriately skilled specialist to directly target the bursitis with very specific an accurate needle placement to administer the steroid pinpoint accurate in the correct structure.
What is the benefit of an ultrasound guided injection?
The traditional way in which steroid injections are administered is through landmark guidance, which means using known landmarks to guide needle insertion. To increase accuracy injections are increasingly administered under ultrasound guidance.
Improved accuracy can reduce the chance of inadvertent needle placement in a neurovascular structure such as an artery or a nerve. This can help to avoid any potential complications. Also increased accuracy of ultrasound guided vs landmark guided injection can improve the outcome of the injection which has been demonstrated in several studies which has been reported by Daniels et al (2018) in their review of the evidence.
The evidence suggest that ultrasound guidance has better outcomes for the: glenohumeral joint, subacromial bursa and biceps tendon. This was also found by several studies involving the hip and knee. There is evidence that for some conditions more accurate needle placement leads to faster benefit and better pain relief (Sibbitt, 2012).
References:
Daniels, E.W., Cole, D., Jacobs, B. and Phillips, S.F., 2018. Existing evidence on ultrasound-guided injections in sports medicine. Orthopaedic journal of sports medicine, 6(2), p.2325967118756576.
Sibbitt WL Jr, Kettwich LG, Band PA, et al. Does ultrasound guidance improve the outcomes of arthrocentesis and corticosteroid injection of the knee? Scand J Rheumatol. 2012;41:66-72
Why should injections be done ultrasound guided?
Why should injections be done ultrasound guided?
Until recently, in most cases injections for musculoskeletal conditions (joints, tendons, ligaments, and muscles) have been done without direct vision of the needle and instead have been carried out based on our knowledge of the anatomy of the structure that we are injecting. Injections based on our knowledge rather than directly visualising the structures that we are injecting are called ‘landmark-guided’ or ‘unguided’ injections.
Some GPs, sports physicians, rheumatologists, orthopaedic specialists, and advanced practice physiotherapists have been carrying out landmark guided injections for many years.
However, accurately delivering an injection, for example, in a tendon sheath or in a joint space without direct visualisation is quite difficult. This is why more clinicians have started using ultrasound guidance to target the injections accurately.
What are the main benefits of ultrasound-guided injections for patients?
- Studies have shown that ultrasound guidance reduces the risks.
- Reduced overall side effects
- Better patient comfort
- Better patient satisfaction
- Significantly more accurate injection with all injection procedures
- Improved outcomes.
How is an ultrasound-guided injection done?
Ultrasound-guided injections should be done in a clean environment with the use of sterile ultrasound gel which is placed on the skin. The ultrasound probe is placed on the gel allowing the operator to see the target structure. The tip of the needle is then carefully advanced while monitored. Next, the needle’s tip is precisely positioned inside the target structure. Once we are satisfied with the accuracy of the needle placement the substance in the syringe (steroid, local anaesthetic and/or hyaluronic acid) can be injected.
Why do I need an ultrasound guided injection?
Pain from joints, ligaments and tendons can affect your quality of life and prevent you from doing normal day to day activities. If symptoms do not respond to conservative treatments (rest, physiotherapy) then an injection of local anaesthetic and steroid can be used to provide pain relief.
Who carries out the ultrasound and injection?
The examination will be performed by a practitioner specialised in musculoskeletal problems (such as a specialist physiotherapist a specialist doctor or a radiologist).
It can take many years to learn how to do an ultrasound injection. As ultrasound guided injections are a difficult skill to master it is important that you find a practitioner who has excellent skills. Those with high levels of skills often are the ones teaching other practitioners to become competent in ultrasound guided injections.
It is important to be able to trust the degree of skill of your practitioner as the use of diagnostic ultrasound and ultrasound guided injections in the UK happens without clearly enforced regulation. This is why at Sonoscope injections are carried out by a practitioner who delivers 1000s of injections per year and who is an experienced lecturer and teacher of ultrasound guided injections both privately and through university (Brunel).
How does it feel to have an injection of local anaesthetic/steroid medication?
To perform the scan a small amount of gel is applied to the skin surface in the area being examined. The skin at the site of injection will be cleaned using an antiseptic solution.
A needle will be put into the area to be treated and the local anaesthetic and/or steroid will be injected. You may feel some pushing as the needle goes in and it will feel heavy/tight as the medication is injected.
You may be asked to wait fora short while after the injection to make sure that you do not have a reaction to the medication used.
Is an ultrasound-guided injection better than an unguided injection?
A recent Umbrella Review and Meta-analysis from Peng-Chieh et al. (2024) ultrasound significantly improved the accuracy of injections, especially
in areas like the bicipital groove, wrist, hip, and knee, leading to better pain relief. They concluded: Ultrasound emerges as a promising tool for enhancing
injection precision and patient outcomes in musculoskeletal pain management. they particularly found that injections into the bicipital groove, wrist, hip,
and knee were yielding greater accuracy and improved pain management.
Another recent systematic review and meta-analysis (ElMeligie, 2022) on the effectiveness of ultrasound-guided versus landmark corticosteroid injection in the treatment of shoulder pain US-guided CS injections showed significant improvement in pain and functional scores (VAS, shoulder functional scores, and shoulder abduction degree) but no difference in disability scores compared with landmark injections.
A review of the existing evidence on ultrasound guided injections (Deng, 2018) summarises: “Given the improvements in accuracy, ultrasound-guided injections certainly have a role for deeper anatomic structures, for injecting targets that are close to large vascular structures, and for patients in whom nonguided injections have failed”.
Conclusions:
Ultrasound guided injections are more accurate than unguided injections. the evidence also suggests improved relief and functional scores. From a safety perspective alone, they should be done in areas with large neurovascular structures and in patients in whom landmark guided injections have failed.
References:
Daniels, E.W., Cole, D., Jacobs, B. and Phillips, S.F., 2018. Existing evidence on ultrasound-guided injections in sports medicine. Orthopaedic journal of sports medicine, 6(2), p.2325967118756576.
Deng, X., Zhu, S., Li, D., Luo, Y., Zhang, X., Tan, Y., Li, J. and He, X., 2022. Effectiveness of Ultrasound-Guided Versus Anatomic Landmark–Guided Corticosteroid Injection on Pain, Physical Function, and Safety in Patients with Subacromial Impingement Syndrome: A Systematic Review and Meta-analysis. American Journal of Physical Medicine & Rehabilitation, 101(12), pp.1087-1098.
ElMeligie, M.M., Allam, N.M., Yehia, R.M. and Ashour, A.A., 2022. Systematic review and meta-analysis on the effectiveness of ultrasound-guided versus landmark corticosteroid injection in the treatment of shoulder pain: an update. Journal of Ultrasound, pp.1-12.
Peng-Chieh, S.H.E.N., Ting-Yu, L.I.N. and Wei-Ting, W.U., 2024. Comparison of Ultrasound-vs Landmark-Guided Injections For Musculoskeletal Pain: An Umbrella Review. Journal of rehabilitation medicine, 56, p.40769.
Cortisone Injections for Osteoarthritis
Relieving joint pain caused by arthritis is the most common reason people are coming to our clinic to have an ultrasound-guided injection. Unfortunately, arthritis and its variants of osteoarthritis and rheumatoid arthritis will eventually affect everyone.
What is arthritis?
The term arthritis literally means inflammation or swelling of the joints. According to the Arthritis Foundation, arthritis is a general term that is used to describe over 100 conditions that affect over 8.5M people in the U.K. These conditions have similar symptoms of pain, swelling, and stiffness of the joints and surrounding areas. The two most commonly diagnosed types of arthritis are osteoarthritis and rheumatoid arthritis.
What is Osteoarthritis?
Osteoarthritis, the most common form of arthritis, is degenerative arthritis. Osteoarthritis commonly affects portions of the wrists, ankles, fingers, and toes, as well as the knees, hips, neck, and lower spine.
The arthritic pain described by osteoarthritis patients includes morning stiffness and stiffness following the inactivity of the affected joint. This stiffness rarely lasts for more than 30 minutes. As osteoarthritis progresses, patients report arthritic pain with movement of the joint and resolution of pain upon resting the joint. In advanced disease, patients report pain at rest and pain that awakens them from sleep.
What is rheumatoid Arthritis?
Rheumatoid arthritis, the second most common form of arthritis, is the chronic swelling and inflammation of the joints. The hallmark rheumatoid arthritis symptom is pannus-a swelling and overgrowth of rough tissue (called granular tissue) over the smooth connective tissue that surrounds the area around and between the bones and joints. Although some cases of rheumatoid arthritis are mild, this type of arthritis is often chronic and progressive and leads to deformities and disability.
What are the risk factors and causes of arthritis?
Although researchers have been searching for the cause of arthritis for decades, the cause of arthritis remains unknown. There are three promising theories about the cause of arthritis. These include:
- Genetic or hereditary factors
- Immune system abnormalities or autoimmune disease
- A persistent or triggering infection.
Because more women have arthritis than men, some scientists believe there is a hormonal component to the disease as well.
Other arthritis risk factors are:
- Age: With the exception of juvenile rheumatoid arthritis, arthritis symptoms often begin after age 40.
- Gender: Women are at higher risk of arthritis. Of the 21 million Americans with osteoarthritis, 16 million of them are women. Other forms of arthritis, including rheumatoid arthritis, lupus and fibromyalgia, occur more often in women than in men. Men have a higher risk of gout (another common arthritis), and they experience osteoarthritis in greater numbers after age 55.
- Weight: As few as 10 extra pounds can translate into a higher risk for arthritis, especially in weight-bearing joints like the knees. This increased weight places more pressure on joints and causes the cushioning layer between bones in a joint (cartilage) to break down.
- Past injuries: A severe joint injury, such as a knee injury that damages cartilage, can add to the overall risk of arthritis.
- Ethnicity: Ethnic background affects the risk of arthritis. For example, 25% of Caucasians carry the genetic marker for rheumatoid arthritis compared to 10% of African Americans.
What are the symptoms of arthritis?
Because there are 100 conditions* that fall under the term arthritis, it would be difficult to list the symptoms of all of them. However, many of the conditions share similar symptoms. Rheumatoid arthritis symptom list:
- Gradual onset
- Weakness, fatigue, and loss of appetite (anorexia)
- Joint swelling, tenderness, and loss of motion, especially in the wrists, ankles, and fingers
- Dislocations and joint contractures
- Chronic inflammation of tendons
- Possible tendon rupture
- Rheumatoid nodules over bony areas such as the elbow and wrist.
- Enlarged spleen
- Pericarditis (inflammation of the heart wall), and vasculitis (inflammation of the blood vessels)
Osteoarthritis symptom list:
-
- Stiffness, pain, and a noisy grating of the joints (crepitus)
- Joint tenderness, swelling
- Decreased range of motion
- Crepitus with motion
- Bony overgrowths
- Pain with movement
- Finger joint involvement leads to the development of nodular swellings.
How is arthritis diagnosed or evaluated?
It is important to see a doctor to be diagnosed properly. Because there are so many types of arthritis, it may take some time to get the correct arthritis diagnosis. Successful diagnosis depends on patient history, symptoms, blood tests, physical examination, and X-rays or radiographic studies. There are no definitive laboratory tests for osteo or degenerative arthritis. Blood work for osteoarthritis is usually normal or inconclusive. A blood test for rheumatoid factor, an autoantibody found in the blood of people with rheumatoid arthritis, can help with a diagnosis of rheumatoid arthritis. X-rays can help with an arthritis diagnosis. An X-ray of an arthritic joint will show joint space narrowing, new and abnormal bone formation, and abnormal, dense tissue growth.
Because many types of arthritis develop slowly, a doctor may suspect one kind of arthritis before other symptoms make the diagnosis clear. Patients should develop a rapport with their doctors and keep a diary of arthritis symptoms to help with diagnosis.
What are the treatments and drugs to treat arthritis?
The goals of arthritis treatment are simple:
- Relief arthritis pain
- Minimize joint stiffness
- Reduce inflammation
- Preserve muscle and joint function
- Maintain a normal lifestyle
- Minimize side effects of arthritis medication.
A basic common sense approach achieves these goals for a majority of patients. Although this approach is not an arthritis cure, it helps patients maintain their quality of life. This arthritis treatment approach consists of
- adequate rest
- anti-inflammatory therapy
- physical therapy to maintain joint function
- drug therapy to slow the progression of the disease (in some patients).
One of the most important aspects of arthritis relief is the control of inflammation and pain. Nonsteroidal anti-inflammatory drugs (NSAIDs) help control these symptoms. There are several types of these arthritis medicines. Some of these medicines are safer to use than others.
NSAIDs include salicylates, traditional NSAIDs and COX-2 inhibitors. Aspirin is a salicylate. Traditional NSAIDs are medicines like over-the-counter Motrin, Advil, and other ibuprofen-containing brands and Aleve and other naproxen/naproxen sodium-containing brands. Other drugs in this NSAID class include ketoprofen, flurbiprofen, oxaprozin, nabumetone, tolmetin, indomethacin, sulindac, piroxicam, diclofenac, diflunisal, and etodolac. Aspirin and NSAIDs can cause GI upset, bleeding and ulcers in some patients.
COX-2 inhibitors are newer agents which bind only to COX-2 receptors. COX-2 inhibitors are less likely to cause GI symptoms than traditional NSAIDs. However, COX-2 inhibitors may not be safe choices for all patients. Recently, Vioxx, a popular COX-2 inhibitor, was removed from the market due to increased risks of stroke and heart attack with long-term use. Another COX-2 inhibitor, Bextra, may cause similar side effects. Celebrex, a third COX-2 inhibitor, may be a safer alternative.
It is important to remember that these drugs do not modify the progression of the disease but simply help with pain and inflammation, which can significantly improve the patient’s quality of life.
Other types of arthritis medication are disease-modifying antirheumatic drugs (DMARDs) such as hydroxychloroquine, gold, penicillamine, the immunosuppressive agent methotrexate, and azathioprine. These drugs can help slow the progress of the disease. Because these drugs have severe side effects for some patients, it is important that the patient be followed closely by their physician.
Steroid injections
Sonoscope offers injections of a long-acting steroid that may be given directly into a particularly painful joint, especially the knee or thumb. The injection often starts to work within a day or so and may improve pain for several weeks or months. Steroid injections are mainly used for very painful osteoarthritis or for sudden, severe pain caused by crystals in the joint.
How is cortisone injection administered?
Cortisone injections are most commonly given into joints to provide pain relief. They can also be given into tendons near the joint (tender points). The cortisone is injected directly into the painful joint with a needle and syringe. Ultrasound may be used to guide the needle into the correct position.
You will usually have the injection while you’re awake, although you may be given a sedative first if you’re anxious. The skin over the injection site is numbed with a local anaesthetic before the cortisone is injected.
Cortisone injections usually take a few seconds to administer. You will usually be able to go home soon after having the injection.
Conclusion
No one arthritis medicine’s best for all patients. Each patient responds differently to each medication. Some doctors prescribe an alternative arthritis remedy such as acupuncture to help control pain. In a recent study, acupuncture worked better than arthritis medication for the control of the pain and swelling of osteoarthritis of the knee.
Regular exercise and appointments with a physical therapist can help preserve a range of motion for arthritis patients and delay disability.
Other aspects of arthritis treatment can include simple interventions such as the local application of heat or ice, periods of rest at selected times during the day, exercise to maintain joint motion and muscle power, and reduction of weight on painful joints by the use of canes or crutches. Patients also need patient education and emotional support. Surgical procedures may be necessary in patients with severe hip or knee involvement or spinal nerve compression.
Sources:
Acupuncture as a complementary therapy to the pharmacological treatment of osteoarthritis of the knee: randomized controlled trial. British Medical Journal. 18 November 2004; 329: 1216-9.
Arnett, FC. Rheumatoid Arthritis. IN: Cecil Textbook of Medicine, 21st ed. Philadelphia, PA: W. B. Saunders Company; 2000: 1492 – 1499.
Arthritis Foundation. What is Arthritis? Available at: http://www.arthritis.org/resources/gettingstarted/what_is_arthritis.asp.
Accessed November 18, 2004.
Arthritis Foundation. Arthritis. What Are The Risks? This content was formerly available at arthritisfoundation.org (link no longer active). For updated information, please see: https://www.arthritis.org/search/results?query=risks
Bathon, JM and Ling, SM. Osteoarthritis. IN: Rakel, MD. Textbook of Family Practice, 6th ed. Philadelphia, PA: W. B. Saunders Company; 2002: 1044-1048.
Mercier, LR. Arthritis, Rheumatoid. IN: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2005 ed. St. Louis, MO: Mosby, Inc; 2005: 89.
Mercier, LR. Osteoarthritis. IN: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2005 ed. St. Louis, MO: Mosby, Inc; 2005: 578.
Stedman, TL. Stedman’s medical dictionary. 26th ed. Baltimore, MD: Williams & Wilkins; 1995: 149.
What is a Musculoskeletal Ultrasound
If you’re looking for a non-invasive way to get a detailed look at your musculoskeletal system, ultrasound is a great option. This imaging modality uses high-frequency sound waves to produce images of the inside of your body, and it can be used to evaluate a variety of conditions affecting the muscles, tendons, and joints. MSK ultrasound can also be used to accurately guide steroid injections in the joints.
What is musculoskeletal ultrasound?
Musculoskeletal ultrasound is a diagnostic imaging technique that uses sound waves to produce images of the bones, joints, and soft tissues such as ( muscles, tendons, ligaments, nerves etc) of the body. It is used to evaluate a wide variety of conditions, from sports injuries to arthritis.
While X-rays and MRI (magnetic resonance imaging) are also used to image the musculoskeletal system, ultrasound has several advantages. It is non-invasive (no needles or injections are required), does not use ionizing radiation (so it is safer for children and pregnant women), and can be performed on an outpatient basis. In addition, ultrasound images can be acquired in real time, which means that the examination can be tailored to the specific condition being evaluated.
How can musculoskeletal ultrasound help diagnose conditions?
Musculoskeletal ultrasound can help diagnose a wide variety of conditions, including:
-Tendinitis
-Bursitis
-Arthritis
-Dislocations
-Muscle tears
-Ligament tears
-Fractures
What are some of the benefits of musculoskeletal ultrasound?
Musculoskeletal ultrasound (MSK ultrasound) is a type of diagnostic imaging that uses high-frequency sound waves to produce detailed images of the joints, muscles, tendons, and other soft tissues.
MSK ultrasound is often used to evaluate problems such as joint pain, muscle pain, or tendonitis. It can also be used to guide needle biopsies and steroid injections.
MSK ultrasound is generally safe and does not use ionizing radiation ( unlike X-rays or CT scans). It is also relatively inexpensive and can be performed on an outpatient basis.
Some of the benefits of MSK ultrasound include:
-It is noninvasive and does not use ionizing radiation.
-It is relatively inexpensive.
-It can be performed on an outpatient basis.
-It can provide detailed images of the joints, muscles, tendons, and other soft tissues.
How is musculoskeletal ultrasound used to treat conditions?
Musculoskeletal ultrasound is used to diagnose and treat a variety of musculoskeletal conditions. The ultrasound waves can help to identify problems with tendons, ligaments, muscles, and joints. The ultrasound waves can also be used to deliver therapeutic treatments such as pain relief or physical therapy.
What are the risks associated with musculoskeletal ultrasound?
Musculoskeletal ultrasound is a safe and effective imaging modality. There are no known risks associated with the use of ultrasound.
What are the side effects of musculoskeletal ultrasound?
Most patients do not experience any side effects from having a musculoskeletal ultrasound. The ultrasound gel used during the exam is cool and does not usually cause any discomfort. If you have a sensitive skin condition, you may want to ask the technologist to use a hypoallergenic gel.
The ultrasound waves used during the exam are safe and have no known side effects. In very rare cases, patients may experience a feeling of warmth or tingling during the exam. If this occurs, please let the technologist know so they can adjust the machine.
How can I prepare for a musculoskeletal ultrasound?
You don’t need to do anything special to prepare for a musculoskeletal ultrasound. You can eat and drink normally before the test.
What should I expect during and after a musculoskeletal ultrasound?
You will be asked to lie on a padded table. A clear gel will be applied to the area of your body being examined. The sonographer will gently move a hand-held device called a transducer over the gel. The transducer emits sound waves that bounce off your bones and create echoes. These echoes are converted into electronic signals that are passed to a computer, which produces images of your bones on a screen.
The musculoskeletal ultrasound procedure is usually painless. However, if you have a very sensitive area, you may feel some discomfort when the transducer is pressed against your skin.
After the musculoskeletal ultrasound is complete, you can go about your normal activities. There are no special precautions you need to take.
What is Ultrasound?
If you’re like most people, you probably think of ultrasound as a way to get a picture of your baby during pregnancy. But ultrasound can also be used for other things, like checking out your organs or looking for tumours. In fact, ultrasound is a pretty versatile tool that can be used for all kinds of different medical purposes such as guiding joint injections. So what is ultrasound, exactly?
What is ultrasound?
Ultrasound is sound waves with frequencies higher than the upper audible limit of human hearing. Ultrasound is not different from “normal” (audible) sound in its physical properties, except that humans cannot hear it. This limit varies from person to person and is approximately 20 kilohertz (20,000 hertz) in young adults. Ultrasound devices operate with frequencies from 20 kHz up to several gigahertz.
There are many different uses for ultrasound. For example, ultrasound can be used:
– To produce images of internal organs for medical diagnosis (medical sonography)
– To monitor the flow of blood and to measure heart function (echocardiography)
– To create images of a developing foetus (obstetric ultrasonography)
– To guide needle placement during biopsies and other procedures (interventional ultrasonography)
– To clean teeth (ultrasonic dental cleaning)
– To break up kidney stones (shock wave lithotripsy)
How ultrasound works
Ultrasound is sound waves with frequencies higher than the upper audible limit of human hearing. Ultrasound is not different from “normal” (audible) sound in its physical properties, except that humans cannot hear it. This limit varies from person to person and is approximately 20 kilohertz (20,000 hertz) in healthy young adults. Ultrasound devices operate with frequencies from 20 kHz up to several gigahertz.
How ultrasound works
When ultrasound waves hit an object, they reflect off of it. The time it takes for the waves to bounce back is used to calculate the depth of the object. The waves also change direction when they hit a boundary between two different materials – for example, the tissue interface between muscle and fat – which can be used to produce two-dimensional images.
The benefits of ultrasound
Ultrasound has a number of benefits, both for medical purposes and for other uses.
Some of the medical benefits of ultrasound include:
– Diagnosing problems in unborn babies
– Looking for problems in the heart, liver, kidneys, or other organs
– Guiding doctors during surgery
– Helping to break up kidney stones
– Reducing pain and swelling from injuries
– Treating cancer
Ultrasound can also be used for non-medical purposes, such as:
– Cleaning jewellery and glasses
– Cutting through metal and concrete
– weld outdoor power equipment
Ultrasonic waves are also used in humidifiers and nebulizers.
The risks of ultrasound
While ultrasound is generally considered safe, there are some risks associated with the procedure. One of the risks is that the sound waves could heat up body tissues. This could damage tissue or cause it to swell. These risks are more usually associated with multiple pulsing modes such as Doppler imaging, and high-frame-rate, high-line-density modes. These imaging settings are hardly used when scanning musculoskeletal tissues and if used (colour or power doppler) they are used for very short amounts of time typically less than a minute.
Another risk is that the waves could reflect off of bones or other structures in the body and cause interference in the image. This could make it difficult to get a clear picture of the area being examined.
Ultrasound may also not be recommended for pregnant women or those who are pregnant with twins or more because of the potential risks to the developing foetuses.
How to prepare for ultrasound
Preparation will depend on the type to of ultrasound you are having.
Some ultrasound examinations like musculoskeletal ultrasounds require no preparation when for some other you might have to fast for a few hours or drink water.
What to expect during ultrasound
You must expect different experiences depending on the kind of ultrasound you are having but in general you will lie on your back on an examination table. A clear gel will be put on your abdomen. The gel helps the sound waves from the transducer travel through your skin to your internal organs.
The transducer is a handheld device that emits sound waves and picks up the echoes as they bounce off your organs. The echoes are then translated into images on a monitor that the radiologist or sonographer can interpret.
After the ultrasound
You should be able to go home soon after the procedure.
Further reading
If you want to learn more about ultrasound, there are a few good sources of information:
-The Mayo Clinic has a good overview of ultrasound, including what it is, how it works, and what it can be used for.
-The American Institute of Ultrasound in Medicine (AIUM) also has a good general overview of ultrasound.
-If you’re interested in the history of ultrasound, How Stuff Works has a short article on the origins of ultrasound technology.
What is an Ultrasound guided injection? - Your Questions Answered
An injection of local anaesthetic and steroid can be used to provide symptom relief for painful and/ or swollen joints, ligaments or tendons. The corticosteroids injection procedure can be performed using a blind injection technique or can be guided by ultrasound to pinpoint the exact location requiring treatment.
What is the benefit of ultrasound-guided v blind injection?
For many years (steroid) injections were done unguided. This means that the person injecting purely had to inject based on his/her knowledge of anatomy and without the direct vision of the needle in the tissue.
Injecting, however into joints, tendon sheaths, and bursas can be quite difficult, especially without the direct vision of the needle.
The image-guided injection can therefore help to make sure that injections are administered accurately and inside of the structure that we want to inject rather than into nearby structures that are not the target of the injection.
Before the wide spread of ultrasound machines, X-ray guidance was the only option. As X-ray equipment is only available in hospitals, it was not easy to access for many people. X-ray guidance also involves radiation which is not ideal. So unless the injection is done for difficult-to-access spinal problems (neck and back), it is now often done under ultrasound guidance.
It is now possible to perform injections using ultrasound to guide the needle in a clinic environment (like a consultation or treatment room) without having to go into the hospital to have it done. This saves money on unnecessary hospital visits and it makes it possible to perform these injections in one session without the need for onward referral to other specialists.
How is an ultrasound-guided injection performed?
A diagnostic ultrasound scan is carried out to identify the structure to be injected (for example, a tendon sheath or a joint or a bursa).
We then clean the skin. Following that sterile ultrasound gel is placed between the ultrasound probe and the skin. This allows us to obtain an image of the joint, bursa or tendon sheath to be injected.
The needle is then carefully inserted and directed towards the structure in need of injection. The needle tip can be placed pinpoint specific exactly where the injection is required.
The video below demonstrates an ultrasound-guided hydrodistension injection for the shoulder joint. Please note how the injection is accurate and the fluid (the injected steroid and anaesthetic) is seen inside of the joint capsule.
Ultrasound guided hydrodistension injection for frozen shoulder
Who performs the ultrasound and injection?
Ultrasound guided injections are usually performed by a consultant radiologist or a specialist sonographer or MSK specialist clinician. In the sonoscope clinic they are performed by a dual trained Advanced Practice Physiotherapist (APP) AND Musculoskeletal Sonographer). The practitioner will explain what happens and will show you what to do.
I am currently taking medication to thin my blood. Do I need to do anything differently?
If you are taking blood thinning drugs, including warfarin, aspirin, clopidogrel, dabigatran, apixaban, rivaroxaban, edoxaban or dipyridamole, please inform us as soon as possible so that we can give precise advice and we can then decide whether or not it is still ok for you to have an injection.
What does the examination involve?
On arrival, you will be asked to remove some of your clothing. If you are attending for your leg you will need to remove clothing that covers your legs (you dont have to remove your underwear. If you are attending for a shoulder examination, you will need to remove your bra strap on the side being examined.
Once in the examination room, you will lie on a couch next to the ultrasound machine.
The specialist will perform the scan by placing a small amount of clear gel onto the skin and gently running a small probe, like a microphone, over the skin surface.
You may be asked to change your position slightly.
The doctor / health professional who arranged for you to have this examination might have asked the practitioner to consider giving an injection which in some cases my be for diagnostic purposes. In most cases there is a dual purpose ie: or both diagnostic as well as therapeutic reasons. The specialist sonographer and Musculskeletal expert will explain whether an injection is necessary once they have scanned the area.
The injection, if necessary, will be of local anaesthetic and/ or steroid medication.
The Radiologist will answer any questions you have about the injection at the time. If you have concerns before the test, please contact the doctor who you saw in the clinic who will be able to discuss the injection further with you.
What are the risks of an ultrasound-guided injection?
Ultrasound uses sound waves and therefore is considered to be a harmless method of imaging the body. There are no known side effects from diagnostic ultrasound scanning. An ultrasound-guided injection is considered a relatively safe procedure which is low risk. Using ultrasound to guide the needle reduces the chances of causing damage to surrounding structures. Side effects related to the procedure include bleeding, infection, numbness/weakness and allergic reaction to the medications used. Please also see our injection information leaflets which will give more detailed information on risks and side effects.
When will I notice a result from the injection?
The local anaesthetic injected may give immediate pain relief and can last for up to 24 hours. The steroid can take several days to take effect and the maximum effect from the injection can take up to 7-10 days. Within two weeks, we will send a report to your doctor.
Can I drive home?
We advise you not to drive for 24 hours after injection and you should make alternative travel arrangements.
Ultrasound-guided injection vs unguided injection what is better?
Many of the studies on corticosteroid injections using ultrasound guidance have shown accuracy superior to that of landmark-guided injections (Daniels et al, 2018).
The efficacy (benefit to patients) and cost-effectiveness of ultrasound-guided injections is less conclusive. This may be due in part to a lack of high-quality research proving the effectiveness of corticosteroids or other modalities to treat many of the conditions for which they are used. (Daniels et al, 2018).
Ultrasound-guided Shoulder injections
The evidence does indicate that for common conditions affecting the shoulder joint such as Frozen shoulder of the shoulder joint (glenohumeral joint), and for conditions affecting the subacromial bursa (subacromial bursitis) ultrasound guided injections are not only more accurate but also more effective.
Ultrasound guided hip Injections
Ultrasound-guided hip injections are 97-100% accurate compared with landmark-guided accuracy of only 66.7-77.5% (Dıraçoğlu, 2009). Hoeber et all (2016), in their systematic review on ultrasound-guided vs landmark-guided injections, concludes that due to the much higher accuracy of ultrasound-guided injections, hips should be injected under ultrasound guidance.
In the meantime Daniels et al (2018) conclude that given the improvements in accuracy, ultrasound-guided injections certainly have a role to play for deeper anatomic structures, for injecting targets that are close to large vascular structures, and for patients in whom nonguided injections have failed.
Ultrasound-guided knee injections
Berkoff et al, (2012) in their review paper found that accuracy was 95.8% with ultrasound guidance versus 77.8% without ultrasound guidance. Sibbitt et al (2011) showed greater accuracy with ultrasound-guided injection. This study also concluded that ultrasound guidance improves clinical outcomes by increasing therapeutic duration.
Who can inject ultrasound guided?
Generally, only people who are skilled in ultrasound diagnostics would perform ultrasound-guided injections. Good practitioners have followed an intensive university CASE accredited PgCert in musculoskeletal ultrasound
It is a difficult skill to master, it can take a good number of years before a practitioner is competent. As a general rule, the people that are highly skilled injectors are those that carry out many injections as an integral part of their work. Frequently these practitioners work in radiology departments where they are surrounded by other experts in musculoskeletal ultrasound, so they are up to date with the latest knowledge and skills in this field. They teach others and share knowledge with colleagues.
Statistics
1. Ultrasound-guided injections are more accurate than blind injections, with a success rate of 97% compared to 83% for blind injections.
2. The success rate for ultrasound-guided injections increases to 99% when the operator has more than five years of experience.
3. Ultrasound-guided injections are less painful than blind injections, with a pain score of 2.3 out of 10 compared to 4.0 for blind injections.
4. The majority of patients (91%) prefer ultrasound-guided injections to blind injections.
5. Ultrasound guided injections are more expensive than blind injections, with an average cost of $50-$100 compared to $20-$50 for blind injections.
6. The majority of insurance companies cover the cost of ultrasound guided injections.
7. Ultrasound guided injections take longer than blind injections, with an average time of 15-20 minutes compared to 5-10 minutes for blind injections.
Summary:
Unguided injections – injections without the direct vision of the needle- are inaccurate compared with ultrasound-guided injections. Ultrasound-guided injections can help to improve injection safety by avoiding damage to critical structures such as blood vessels and nerves. They are generally also less painful than unguided injections.
Ultrasound-guided injections are not easy to learn, and it can take years for practitioners to be competent.
The lead clinician at Sonoscope (Robert Mast) has many years of extensive experience in musculoskeletal ultrasound. He also works in a radiology department and does many diagnostic ultrasound scans. He safely and accurately administers many injections. He is an honorary lecturer at Brunel University, where he teaches diagnostic ultrasound and ultrasound-guided injections.
Berkoff, D.J., Miller, L.E. and Block, J.E., 2012. Clinical utility of ultrasound guidance for intra-articular knee injections: a review. Clinical interventions in aging, 7, p.89.
Daniels, E.W., Cole, D., Jacobs, B. and Phillips, S.F., 2018. Existing evidence on ultrasound-guided injections in sports medicine. Orthopaedic journal of sports medicine, 6(2), p.2325967118756576.
Dıraçoğlu, D., Alptekin, K., Dikici, F., Balcı, H.İ., Özçakar, L. and Aksoy, C., 2009. Evaluation of needle positioning during blind intra-articular hip injections for osteoarthritis: fluoroscopy versus arthrography. Archives of physical medicine and rehabilitation, 90(12), pp.2112-2115.
Hoeber, S., Aly, A.R., Ashworth, N. and Rajasekaran, S., 2016. Ultrasound-guided hip joint injections are more accurate than landmark-guided injections: a systematic review and meta-analysis. British Journal of Sports Medicine, 50(7), pp.392-396.
Sibbitt Jr, W.L., Band, P.A., Kettwich, L.G., Chavez-Chiang, N.R., DeLea, S.L. and Bankhurst, A.D., 2011. A randomized controlled trial evaluating the cost-effectiveness of sonographic guidance for intra-articular injection of the osteoarthritic knee. JCR: Journal of Clinical Rheumatology, 17(8), pp.409-415.
Patient experience of hydrodistention injection for frozen shoulder
Pain and discomfort from a frozen shoulder is one of the most common reasons patients get in touch with us, so I thought it might be helpful for people to hear directly from a patient what it is like to receive a hydrodistension injection for a frozen shoulder.
If you would like to know more about this condition, please visit our frozen shoulder treatment page.
I performed a hydrodistension procedure for Rebecca’s frozen shoulder approximately 6 weeks ago. The total volume injected was 20ml before capsular rupture.
I recently asked her to describe what it is like to have a frozen shoulder injected with a high volume. I also wanted to know her progress.
Below is her account:
WHAT WAS THE REASON THAT YOU WERE GIVEN A HYDRODISTENSION INJECTION?
A three-month-old frozen shoulder
CAN YOU DESCRIBE THE PROCEDURE? (WHATEVER YOU CAN REMEMBER OF IT).
After explaining what he had seen on the ultrasound scan, Robert inserted the needle into the back of my shoulder and talked me through the procedure as he inserted 5ml fluid into the joint space, I felt a fullness in the shoulder joint/capsule, and Robert then asked if I felt he could inject more fluid in after I agreed he was able to inject another few ml before I felt a pop as the capsule released.
WAS IT PAINFUL?
It was uncomfortable, however, the main feeling was a fullness of the shoulder, it felt as though the joint was going to burst
WERE YOU ADVERSELY AFFECTED IN YOUR DAY-TO-DAY ACTIVITIES IMMEDIATELY AFTER THE INJECTION?
No adverse effects at all.
HOW LONG AFTER THE INJECTION DID YOU FIRST FEEL THE BENEFIT?
Pain reduction over the first week and movement increased over the following 5-6 weeks.
HAS THE INJECTION MADE A DIFFERENCE IN YOUR DAY-TO-DAY ACTIVITIES?
A significant functional improvement would not have been possible without the intervention.
HAS YOUR SHOULDER IMPROVED FURTHER OVER THE WEEKS /MONTHS SINCE THE INJECTION? PLEASE DESCRIBE IN WHAT WAY:
Increased range of movement, strength and function over the following 5 weeks.
Other Posts that might be of interest
Can You Drive After a Steroid Injection?
October 21, 2025
Frozen shoulder and injection therapy
May 24, 2025
ITB friction syndrome
April 24, 2025
Guidelines for Frequency of Steroid Injections
March 5, 2025