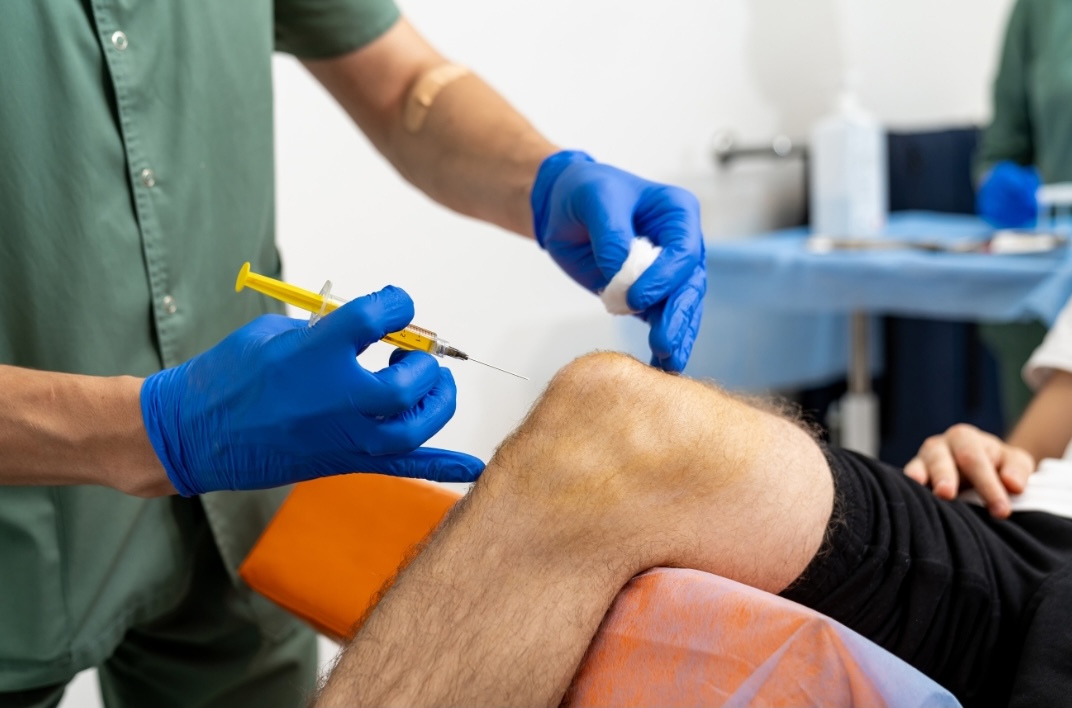
Guidelines for Frequency of Steroid Injections
Steroid injections are generally used to reduce inflammation and pain.
We will look at the guidance on the frequency of these injections. There is some evidence from studies on people with rheumatoid arthritis suggesting that multiple steroid injections in the same joint are safe to administer (1). However, injection therapy frequency must be seen in the context of the individual patient. In very young patients, repeat injections are avoided, if possible, given their young age and the possibility that more injections could be required, and only a finite number of repeat injections can be given.
However, there may not be any other treatment options available for elderly patients, such as those with severe pain and/or dysfunction, especially if a previous steroid injection has been administered and was successful for a long time.
There are limitations to the maximum frequency of steroid injections that can be given. It is generally accepted that no more than 3 steroid injections in any one joint should be given per year.
Again, context is everything here. I think that many practitioners would hesitate to do 3 injections/year every year in perpetuity. And again, in young people, most would agree that it is inappropriate to continue with repeat steroid injections x 3 in the same joint year after year. Even in older patients, most practitioners would also be quite careful, but if no other options exist and the patient does get very good pain relief, then in some instances, more than 3 in total might be given.
Another factor to consider is the amount of time between injections that should be allowed before a repeat steroid injection can be administered. NHS guidelines https://www.nhs.uk/conditions/steroid-injections/ suggest that there should be a 3-month gap between steroid injections, although context is everything here and in specific cases, a steroid injection given after 6 weeks might be acceptable.
Side-effects: It is well-known that long-term, excessive use of steroid injections can lead to significant structural damage such as: Thinning of the soft tissue and skin and muscle tissue, weakening of cartilage and bone, increase the risk of joint infection and possible increased glucose levels leading to diabetes. Please also see this link to a post on the side effects of steroid injections.
- Combe B. Early rheumatoid arthritis: strategies for prevention and management. Best Pract Res Clin Rheumatol. 2007;21: 27-42.
The Role of Steroid Injections in Treating Arthritis
Steroid Injections in Treating Arthritis
Steroid injections are commonly used in musculoskeletal conditions such as osteoarthritis. However, they can also play an important role in managing joints affected by inflammatory arthritis such as Rheumatoid arthritis or psoriatic arthritis or conditions such as gout.
Through complex processes, steroids have powerful anti-inflammatory effects, which help to reduce the levels of inflammation of the joint in question. Pain levels will improve with the reduction in inflammation. The mechanism of action leads to a decrease in synovial blood flow and the number of leukocytes, as well as the release of inflammatory mediator (1). Joint inflammation in knee OA is associated with progression of cartilage damage, therefore steroid injection might reduce disease progression.
As indicated above, inflammation causes swelling and pain. Steroid injections, therefore, can reduce swelling of joints and other structures affected by inflammation. This will help with mobility and function.
It is well-known that steroid injections have a temporary effect, but this can last for a good number of months. It is therefore not uncommon that for those with self-limiting conditions such as: Frozen shoulder, certain degrees of tendinopathy and bursitis etc. a single steroid injection might be sufficient for the problem to disappear completely and for it to never return. The reason for this is that natural healing will take place, and by the time that the steroid has stopped working the person has recovered naturally.
Of course, for more chronic conditions with significant structural damage, such as significant degrees of osteoarthritis, the benefit of the steroid injection is often more temporary in nature although from experience I have found that in a good number of cases the steroid helps to settle the acute pain for months at which point the joint might have settled naturally in a state where pain is no longer a significant issue despite the fact that the degenerative changes present are still unchanged.
In the case of osteoarthritis if someone does require repeat injections, they may well benefit from hyaluronic acid injections, which contain hyaluronic acid (a natural component of joint fluid). These injections contain a synthetic form of hyaluronic acid and help to lubricate the affected joint.
Rastogi, A.K.; Davis, K.W.; Ross, A.; Rosas, H.G. Fundamentals of Joint Injection. Am. J. Roentgenol. 2016, 207, 484–494.