What is frozen shoulder?
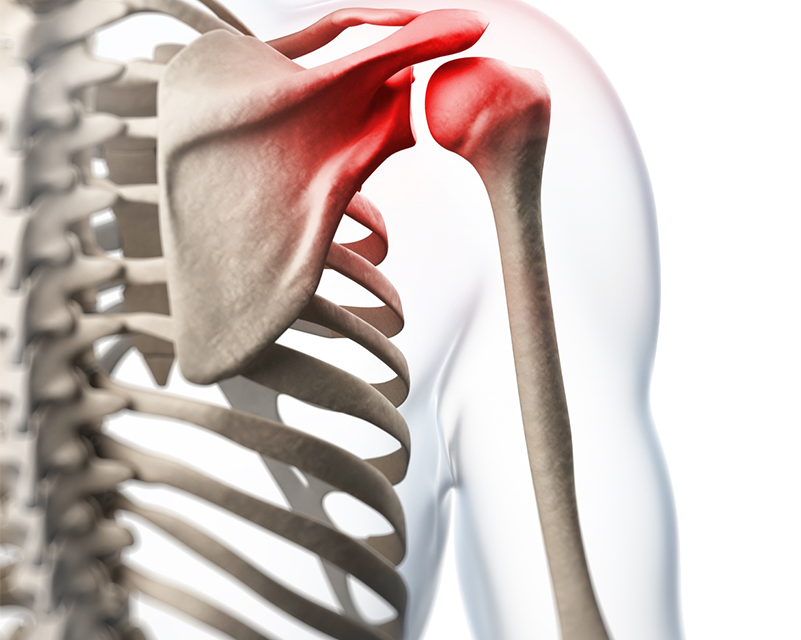
Frozen shoulder is a common condition estimated to affect 2%-5% of the population (Hand, 2008). It is often a condition that develops gradually, and its main feature is of stiffness and pain. The joint that is affected is the glenohumeral joint (from Greek glene which means eyeball, and –oid, refers to ” the form or shape “) i.e. shape of an eyeball. Looking at the image of the skeleton, you can clearly see that shape and form wise, the name makes sense! This is the joint between the humerus (your upper arm bone) and the scapula (shoulder blade).
Injections for Frozen Shoulder: Targeted Cortisone and Steroid Treatments for Effective Pain Relief
In managing frozen shoulder, clinicians often recommend a tailored injection approach that includes either a cortisone injection or a steroid injection directly into the shoulder joint. This method targets inflammation in adhesive capsulitis while significantly reducing shoulder pain. When injections for shoulder conditions are applied with precision, patients tend to experience a noticeable reduction in discomfort, offering a promising alternative to relying solely on physiotherapy.
Advancements in imaging, particularly with ultrasound-guided techniques, have transformed the treatment of frozen shoulder. These ultrasound-guided injections allow practitioners to deliver an accurate dose of corticosteroid and local anaesthetic, ensuring that the medication reaches the affected rotator cuff area and glenohumeral joint with precision. Such targeted delivery is crucial for patients who require a reliable and effective injection to ease pain and restore range of motion.
Furthermore, integrating injections with a comprehensive rehabilitation program is essential. Conservative management through structured physiotherapy and a home exercise program can enhance the effects of a single injection, whether it is a cortisone injection or another variant of intra-articular corticosteroid injections. By combining the benefits of pain relief from the injection with targeted rehabilitation exercises, overall shoulder function can improve, reducing the risk of future stiffness.
For individuals exploring treatment options, it is important to recognize that various shoulder conditions require a personalized approach. Whether addressing the initial stages of a painful condition with a first injection or planning further interventions after a systematic review and meta-analysis of treatment outcomes, healthcare professionals are committed to guiding patients through safe, evidence-based practices. For those experiencing significant pain and stiffness around the shoulder, booking an evaluation may be the first step toward regaining a full range of movement and eliminating shoulder pain.
What are the symptoms of frozen shoulder?
Patients often experience a deep-seated ache in the shoulder, usually at the back of the joint. The pain often radiates down the shoulder in the upper arm. Movements are restricted, usually outward rotation of the shoulder is most affected. Any overhead movements are also restricted. This means that normal day-to-day activities such as getting dressed and combing hair are often affected. Pain at night is another common feature of this condition.
Commonly, three different stages of frozen shoulder are identified:
The freezing stage, which is dominated by pain and thought to be the inflammatory phase, is then followed by the frozen stage, which is the stage that is dominated by stiffness, and eventually, the thawing stage when pain is not so much of a feature, but they are still significant stiffness whilst gradually range of motion returns.

What causes frozen shoulder?
Frozen shoulder is most commonly seen in those between the ages of 40 years of age and 60 years of age.
Thyroid problems, diabetes, cancer and kidney disease appear to increase the risk of developing a frozen shoulder. Parkinson’s disease and Dupuytren’s disease are also associated with a higher risk of developing a frozen shoulder.
Recent injury to the shoulder, which could have been trivial, can also increase the risk of developing a frozen shoulder.
How long does frozen shoulder last?
Vastamäki (2012) retrospectively reviewed patients diagnosed with frozen shoulders over a period of 27 years. 51 patients had been observed only without treatment. 94% of these patients recovered to normal levels of function and motion without treatment in a period of on average 15 months (range 4-36 months).
How is frozen shoulder diagnosed?
Frozen shoulder is predominantly diagnosed clinically (using a physical examination). The clinical evaluation should be performed by an expert in the musculoskeletal examination. The Sonoscope ultrasound guided injection clinic offers assessment by expert physiotherapists with in excess of 20 years of experience in diagnosing and treating people with frozen shoulders.
An x-ray is a useful examination to identify bony causes of stiffness in the shoulder, such as osteoarthritis, and rule out more uncommon bone pathologies. Whilst x-ray is very good at evaluating bone, it only provides very limited information on soft tissues (muscles, tendons, ligaments etc.).
Ultrasound is very helpful here. Ultrasound can evaluate rotator cuff tendons for tears. It can also evaluate the joint margins for signs of osteophytes, which are very common in osteoarthritis. This is very helpful in combination with the clinical examination.
The ultrasound helps to confirm this diagnosis by ruling out any other conditions such as rotator cuff tear, subacromial bursitis, osteoarthritis, calcific tendinopathy and other conditions that can mimic frozen shoulder. Once this is done, an injection to treat the condition can be performed, usually within the same session.
Frozen shoulder, how do we treat it?
According to a British Medical Journal practice review paper by Rangan (2016) there is limited evidence to suggest that physiotherapy might be helpful to treat frozen shoulder. As exercise does not have known harmful effects it is a good option to start with in addition to watch full waiting.
The only substantial evidence for effective treatment of frozen shoulder is for intraarticular steroid injection and for intra articular hydro dilatation (or hydrodistension) injection and the degree of evidence is classed as moderate.
What treatments does the Sonoscope clinic offer for a frozen shoulder
Here at the Sonoscope Injection clinic, we offer both steroid injections and hydro dilatation or hydrodistension injections. In both cases steroid is injected into the joint, but in hydrodistension injections, a significant amount of salty water is also injected with the aim of stretching the joint and reduce the tightness, which benefits the flexibility of the joint.
Sonoscope provides ultrasound-guided steroid injections that offer better accuracy and results.
References
Hand C, Clipsham K, Rees JL, Carr AJ. Long-term outcome of frozen shoulder. J Shoulder Elbow Surg. 2008;17:231–6.
Rangan, A., Hanchard, N. and McDaid, C., 2016. What is the most effective treatment for frozen shoulder?. Bmj, 354, p.i4162.
Robinson, C.M., Seah, K.M., Chee, Y.H., Hindle, P. and Murray, I.R., 2012. Frozen shoulder. The Journal of Bone and Joint Surgery. British volume, 94(1), pp.1-9.
Shah N, Lewis M. Shoulder adhesive capsulitis: systematic review of randomised trials using multiple corticosteroid injections. Br J Gen Pract 2007;57:662–667.
Vastamäki, H., Kettunen, J. and Vastamäki, M., 2012. The natural history of idiopathic frozen shoulder: a 2-to 27-year followup study. Clinical Orthopaedics and Related Research®, 470(4), pp.1133-1143.

Meet Rob - Our Specialist Physiotherapist/ Sonographer
Rob is a specialist Extended Scope Physiotherapist with more than 20 years experience in managing complex musculoskeletal conditions.
He uses diagnostic ultrasound as an extension of his clinical skills. He is an interventional sonographer in a busy radiology department of a central London Foundation Trust Hospital .
Also make sure you check out our Facebook and Youtube channels to keep up to speed with our latest news
